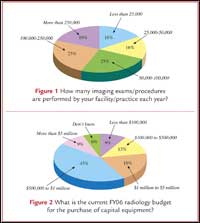
|
The ability of positron emission tomography (PET) to identify otherwise hard-to-detect cancers very early on is making this nuclear medicine modality increasingly popular among referring physicians, patients, the media, and the public. Consequently, more and more hospital radiology departments and freestanding imaging centers are giving serious consideration to adding PET to their service-line retinue. Harry Agress, Jr, MD, director of the Division of Nuclear Medicine in the Department of Radiology at Hackensack University Medical Center, Hackensack, NJ, applauds these radiology enterprises for showing interest in PETadopting it will prove highly beneficial to&them and their various constituencies, he saysbut bringing aboard PET and finding success with it require serious (not to mention strenuous) effort, he hastens to point out.
“PET is fast coming to be seen as a necessary part of the cancer work-up,” Agress says. “The public is beginning to become very cognizant of this, which means that in the future, when they seek cancer treatment and follow-up, they will want to go to only those facilities offering PET. If you don’t have it at your institution, they’ll go someplace else.
“However, PET is not your father’s bone scan. PET is much more complex in terms of time and personnel than you might imagine. Therefore, you cannot approach PET as if it were just another scan. You must instead approach it as you might if you were going to launch and operate a small business. By that, I mean you must have in place solid administrative, marketing, financial, and production components, just as would exist in any small business outside of radiology.”
SEPARATION OF POWERS
For starters, Agress, who oversees PET at Hackensack, contends that a PET service should be run with ledgers and records separate from those of the radiology department (or imaging center) in order to facilitate betterand easierunderstanding of how the PET business is faring.
“It can be difficult to get at the numbers if everything is folded into the books of the larger enterprise,” he warns.
At Hackensack, where dedicated PET service has been established since 2000, having separate figures enables Agress to receive a weekly tally of how many PET scans the unit performed in the previous 7 days, how many scans are scheduled for the coming week, and how many scans are pending receipt of insurance precertification (this latter figure impacts the number of studies that can be performed, since Agress’s policy is to do no test without first obtaining approval from the payor).
“This information is supplied to me on a spreadsheet so I can see the trends and be able to readily and reliably respond to them,” he says.
 Harry Agress, Jr, MD Harry Agress, Jr, MD |
Agress indicates that in a PET venture, “you begin small and then you reach a point where all of a sudden the service catches on. It’s not a point measured by achievement of a certain volume of scans, but it’s a point where a critical mass of people in the community knows about the service, talks about it, and decides that PET is the test they want. When that day arrives, there can be a sudden upswing in demand for PET service. You’ll be inundated with calls from physicians, patients, and insurers. Everything can get very complicated as a result. You have to be prepared for all of this with the proper administrative supportor, at least be able to quickly obtain the additional manpower necessary to handle the increased volume of activity and inquiries.”
A mistake his department made in its early days of PET was to utilize a scheduler who also was tending the appointment logs for the entire nuclear medicine division. This arrangement, says Agress, was embraced to help central scheduling as the PET system had been installed in a location outside the nuclear medicine area.
“Because of this, the scheduling became too much a burden for that one person,” he reveals. “We solved it by installing a separate phone line dedicated to PET and having it answered by a receptionist exclusive to the PET service. What made this necessary was the deluge of PET-related questions the nuclear-medicine scheduler handling the phones soon faced. We did not appreciate how many questions patients and physicians would have about the test. We didn’t anticipate the volume of phone work that would be required.”
After realizing the seriousness of the problem, Agress says he petitioned hospital higher-ups to authorize the addition of extra receptionists. Fortunately, senior Hackensack University Medical Center administrators John P. Ferguson, president and chief executive officer, Robert C. Garrett, executive vice president and chief operating officer, and Barbara Hopkins, vice president of operations, possessed the vision to move forward aggressively with PET.
PET service officially came to Hackensack University Medical Center with gamma camera coincidence imaging in May 1999, 18 months before the nuclear medicine division fired up its dedicated PET scanner . Since installing a dedicated scanner in December 2000, the center has produced more than 2,200 PET scans.
Given the cost of a PET system, an enterprise needs to be able to count on running no fewer than two to three scans every business day to justify the expense of equipment acquisition, Agress says. “If you can generate higher volume than that, then PET should turn out to be a definite financial plus for your enterprise, with the caveat that these numbers could change as reimbursement fluctuates,” he says.
However, in the event such volume is not possible, then Agress recommends building the venture around a mobile PET unit instead. “It’s a very low-risk way to get into PET,” he says. “With mobile you don’t buy the equipment. You merely rent the time slot and the mobile PET operator brings the equipment to your facility aboard a specially outfitted truck and trailer. You can arrange to have the mobile unit parked at your facility 1 day a week and do all your scans at that time.”
Agress says PET is reasonably well reimbursed, but the lion’s share of money collected from payors typically goes to cover the facility component. “For reasons I don’t quite understand, the technologic component for PET can account for well over 90% of the reimbursement, while the professional component is usually only about 5%,” he notes.
PROMOTING THE SERVICE
At least initially, PET requires a big marketing push. According to Agress, promotion should begin 3 to 6 months in advance of the arrival of the equipment and continue robustly after installation. Marketing should target referring physicians, first and foremost.
“Your key referrers will be oncologists, pulmonologists, radiation oncologists, and other radiologistsespecially the ones who read CT scans,” says Agress, who also holds the title of senior attending radiologist in his department. “Important as well are cardiologists, since PET is also an excellent test to determine whether a patient has potentially repairable cardiac tissue in the aftermath of an infarction. To the key referrer list, I also would include general surgeons andbecause of their role as gatekeepers in a managed care environmentprimary-care physicians.”
When the center first offered PET, an announcement notice of the new capability was delivered to prospective referring physicians throughout the hospital. Additionally, Agress conducted grand rounds and made presentations before various tumor boards, enthusiastically touting the PET service each time. “The most effective marketing is one-on-one interaction with the key referrers,” he says.
For purposes of those interactions, Agress recommends that PET presentations be flexibly structured so they can be readily adapted to the interests of each type of referring physician encountered.
“What I did for our PET service was put together a package of selected case studies and copies of pertinent supporting journal articles for the physicians I met withthe studies and articles were specific to the individual physician’s specialty, which made a much stronger impression than if I had provided instead general materials or materials that weren’t connected to his or her area of expertise,” Agress tells.
A technique Agress finds effective when discussing PET with referring referring physicians who are not familiar with the modality’s capabilities entails showing them a CT scan of a cancer patient and asking them to describe how they would handle the management of that particular case, then showing them a PET scan of that same patient and asking whether they would still want to handle the management as first decided.
“The answer they give is frequently no, because the PET scan often shows subtleties and abnormalities not seen or difficult to identify on the CT scan, completely changing one’s thinking about the staging and treatment. It’s a real eye-opener for referring physicians when you lay it out for them in this manner.”
The marketing of PET also should include direct-to-consumer outreach, Agress suggests. “My hospital has its own educational radio program, so we were able to arrange for the airing of an entire segment about PET on one of the health shows,” he says. “We also wrote up a press release that we sent to our local news media. Both were very effective in getting out the word about our service to the public.”
INDICATION GUIDELINES A MUST
After the PET service debuted, Agress says it was not automatic that every oncology patient coming through the nuclear medicine department would receive a PET scan.
“We were very specific about candidates,” Agress says. “Even today, when a physician requests a PET scan, we fax him or her a form to complete and return to us so we can determine whether PET is indicated for the patient in question. The form asks for the patient’s medical history and clinical data as well as anything else that would be vital for us to know. We also ask for a copy of the patient’s most recent prior CT scan along with its report of findings.”
(The CT scan is requested so that the interpreting radiologist can use it to correlate the PET results, a technique that greatly improves the ability to detect abnormalities of concern, Agress explains.)
Agress says he or one of his colleagues in the nuclear medicine division personally reviews and then decides to accept or reject the referring physician-submitted request for a PET scan.
“We have a list of the indications for PET,” he says. “These are mainly lung cancer, colon cancer, lymphoma, head-and-neck cancer, esophageal cancer, melanoma, and solitary pulmonary nodules. Sometimes, referring physicians order PET when one or more of these indications are present, but we decide the test is inappropriate regardless because, for instance, the lesions that show up on the CT scan are too small to merit the expense of a PET scanfor example, a lung nodule of less than 5 mm.”
A characteristic of the indications for PET as developed by Agress and his team is that payors generally have deemed all of them appropriateand reimbursablereasons to run a PET scan.
“There are other indications beyond these that some private insurers will pay for and that Medicare may one day decide to approve,” Agress says. “These include certain thyroid cancers, pancreas cancers, gastric cancers, and some gynecologic tumors. Hopefully, at some point, there will be PET reimbursement approval for evaluation of Alzheimer’s disease.”
Whenever PET is determined to be not indicated, Agress or one of his colleagues in the division calls the referring physician to discuss the reasons for declining the request to test.
“In talking this over with the referring physician, we always recommend he or she continue following the patient with CT so that if, say, the undersized lung nodule gets bigger, we can talk again about imaging it with PET,” Agress explains. “Basically, we want to make sure the right study is performed for each clinical situation. We have no interest in doing PET for patients for whom we don’t think it would be beneficial or for whom it would not change their management.
“We also undertake this review process because we want to make sure that we will be reimbursed for each study. In fact, we’ve made it a policy that we won’t do the PET scan unless it’s precertified by the insurance company or Medicare.” Exceptions include cases of academic interest or pro bono charitable instances.
Responsibility for precertification belongs to the referring physicians, Agress indicates. “We provide some assistance with that in terms of helping the referring physicians’ offices pull together the appropriate documentation,” he says.
THE VALUE OF FOLLOW-UP
Owing to the sophistication of PET imaging, it takes much time and effort to train radiologists in the proper methods of working with the modality and its output.
“PET images have enough variances that make it a little more complex working with them than other types of nuclear medicine scans, so there’s a big learning curve involved,” Agress says. “How far that curve extends will depend on the individual radiologist’s or technologist’s familiarity with nuclear medicine.”
PET vendors typically offer training. Agress urges taking advantage of that.
“Usually, this entails the vendor sending your key radiologist and your chief technologist to a 3- to 5-day-long PET course conducted at one of the major academic centers that has a strong legacy of success with PET,” he says.
Meanwhile, the Society of Nuclear Medicine (SNM) has established a PET learning center to instruct both radiologists and technologists in the nuances of the modality, Agress reports.
“It’s not a substitute for a site visit to a facility where PET is in use, but it offers a tremendous amount of information for a radiologist or nuclear medicine physician who is just getting started with PET,” says Agress, who serves on the faculty of the SNM learning center. The intensive course is held during a single weekend.
Much learning is possible, too, from making a habit of conducting case follow-ups, all the way “to the tissue,” Agress is fond of saying.
“There were times when I wasn’t sure that an abnormality on the PET scan was significant, but by doing follow-up, I was able to have those questions answered,” he says. “Follow-up has given me the ability to look at a PET scan with far greater confidencefor example, abnormalities I might not in the beginning have considered significant, I will now quickly recognize as being significant.”
Agress says he employs a spreadsheet to track cases for follow-up. This contains the name of each physician who referred a patient, the physician’s contact number, the patient’s primary disease, the finding, and what the biopsy or surgery ultimately revealed about the abnormality. The cases Agress chooses for follow-up are typically those that have an interesting or unusual aspect.
“Follow-up also helps focus attention on unexpected problems that otherwise might not be noticed for a long time afterwardand, from the patient’s perspective, it is far better to detect problems sooner rather than later,” he offers. “If you just do the PET scan and give the referring physician a written report, there is a risk that the PET scan will simply become one of many different inputs. But the process of follow-up with personal contact changes that.”
A benefit of conducting follow-up is that it increases the opportunity for interaction with referring physicians, which, not coincidentally, also helps build their confidence in and understanding of the modality. Moreover, follow-up demonstrates to referring physicians that Agress and his team have a serious, ongoing interest in the cases being sent to them, something the referring physicians genuinely appreciate. Stronger relationships result, Agress says.
With regard to advocates, Agress says a successful PET service needs one key physician in the nuclear medicine department or the radiology department at large.
“Right at the beginning, there should be one physician who is very involved in the process of bringing aboard PET and developing it as a business,” he says. “That individual will serve as the point person who gets all the different organizational setup tasks done. Usually, the right person for the assignment is someone who is very excited about PET and believes in it. After the program gets started, it becomes the responsibility of that individual to train several other radiologists to read PET proficiently.”
In Agress’s opinion, there is no question that PET is becoming a major element of the management of oncology patients. However, it does not end there.
“With FDG-PET, we are talking about just one isotope that allows us to do nothing more, really, than look at the distribution of sugar in the body,” he says. “Even now, more radiopharmaceuticals are in development. Just imagine what we’ll be able to do when we have tracers that are specific for individual cancers.”
Rich Smith is a contributing writer for Decisions in Axis Imaging News.