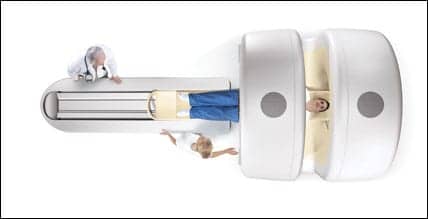
The PRIMATOMTM has found great utility in treating prostate cancer patients: current treatment extends 5 mm beyond the expected microscopic margins of the tumor, but calculations suggest that a 3-mm margin may be adequate. The PRIMATOMTM has found great utility in treating prostate cancer patients: current treatment extends 5 mm beyond the expected microscopic margins of the tumor, but calculations suggest that a 3-mm margin may be adequate. |
Conventional methods of localizing cancers have become increasingly unsatisfactory as computing power has increased the ability of radiation oncologists to tailor radiation fields for three-dimensional conformal radiation therapy and its even more precise forms, intensity-modulated radiation therapy.1 In the past, a tumor was localized during a planning session and then either the skin over the site was tattooed or an immobilizing cast was constructed and marked to indicate the site above the tumor.
Both methods assumed that the tumor-bearing tissue would remain where it had been during the planning session and that the tattooed skin would not move. Neither assumption is correct. James R. Wong, MD, chair of the radiology department, Morristown Memorial Hospital, Morristown, NJ, says, “As people get older, their skins get looser. If the skin moves before you aim the beam at the tattoo, you may miss part of the tumor. Casts would be wonderful if the patient were a block of wood, but people are eating too many hamburgers, so they have a lot of subcutaneous tissue. When the patient moves, the skin, muscle, and fatty tissue conform to the shape of the cast, but they may not be where they were when you did the treatment planning.”
Prostate cancer exemplifies the problems facing the radiation planner. The gland lies between the bladder and the rectum and thus is subject to frequent displacement by their varying degrees of distension. A patient may be told to urinate 15 minutes before the scheduled treatment; can he empty his bladder again if his session is delayed half an hour? “Many people cannot urinate on command,” Wong remarks.
The extent of mobility of the prostate has been documented by Canadian radiation oncologists.2 In a series of 11 patients in whom radiopaque markers were placed before external-beam therapy, images obtained by electronic portal imaging during the treatment session showed marker displacements as large as 1.6 cm from one day to the next. In another series of 35 patients scheduled for brachytherapy, the gland volumes measured at planning and in the operating room before seed implantation were identical in only 37%,3 and in some patients, the difference in volume was as great as 21%. Even when the volume was unchanged, some patients displayed differences in prostate shape. Further complicating the issue is the use of neoadjuvant androgen-ablation therapy in some patients; this treatment shrinks the gland.
Recognizing these problems, some radiation oncologists obtain images of the tumor before each treatment session. It is necessary, in these cases, either to move the patient from the imaging system to the linear accelerator (creating an opportunity for the tumor to move) or to use ultrasonography (which provides less-than-ideal tumor images. A newer alternative avoids both problems.
“After you immobilize the patient on the treatment table, you could take a CT scan to see where the tumor is,” Wong says. “Then you would aim the beam. Because the location of the tumor at that time is known exactly, the beam can be tailored more precisely. This is a simple idea, and it is amazing that it took so long for people to figure it out,” he adds.
Uematsu developed a prototype machine combining CT and a linear accelerator. The initial report from Japan4 described its use for treating brain tumors; there was no need for stereotactic frames. A later paper5 reported use of the device, in combination with beam control and patients’ breath holding, for the treatment of lung cancer. “In 1996, Uematsu and I took the idea of a combination machine to Siemens,” Wong says. The result was the PRIMATOM”. The Carol G. Simon Cancer Center at Morristown Memorial Hospital was the first facility in the United States to install this machine, and it has gained the most extensive experience outside Japan.
The unit, Wong says, “is like a smart bomb. We can guide our treatment exactly to the target. At present, our treatment area extends 5 mm beyond the expected microscopic margins of the tumor, but our calculations suggest that a 3-mm margin may be adequate. The conventional margin is 1 cm.” The PRIMATOM is now used principally to treat tumors of the lung, prostate, and liver. “I believe that we can use the system for many more lesions,” Wong says, “but we have only one PRIMATOM.”
The Simon Cancer Center has been using the PRIMATOM for only 2 years,6 so it is difficult for the facility to determine the influence of imaging immediately before treatment on tumor control and complications. Wong notes, however, that “common sense tells us that if you do not miss the tumor, your kill rate should be higher, and if you treat less normal tissue, your complications should be decreased.” The PRIMATOM uses a diagnostic CT scanner. Although MRI might seem desirable because of its excellent ability to depict soft tissue, it would interfere with the linear accelerator. Other modalities do not provide images with sufficient quality and resolution.
A possible future improvement might be the use of the linear accelerator itself for imaging. This could be accomplished by directing a series of narrow megavoltage or kilovoltage beams at regularly spaced sites on the gantry. The data would then be captured using a large-area, flat-panel, amorphous-silicone electronic portal imaging device7,8 or charge-coupled-devicebased fluoroscopy system9 and reconstructed into a three-dimensional image. The technique, called cone-beam CT, is still in development, but may eventually supersede the hybrid CT scanner and linear accelerator. “Cone-beam imaging is very new,” Wong says. “Eventually, the technology may catch up with diagnostic CT or even replace it.”
Judith Gunn Bronson, MS, is a contributing writer for Decisions in Axis Imaging News.
References:
- Saw CB, Ayyangar KM, Zhen W, Yoe-Sein M, Pillai S, Enke CA. Clinical implementation of intensity-modulated radiation therapy. Med Dosim. 2002;27:161-169.
- Vigneault E, Pouliot J, Laverdiere J, Roy J, Dorion M. Electronic portal imaging device detection of radioopaque markers for the evaluation of prostate position during megavoltage irradiation: a clinical study. Int J Radiat Oncol Biol Phys. 1997;37:205-212.
- Beaulieu L, Aubin S, Taschereau R, Pouliot J, Vigneault E. Dosimetric impact of the variation of the prostate volume and shape between pretreatment planning and treatment procedure. Int J Radiat Oncol Biol Phys. 2002;53:215-221.
- Uematsu M, Fukui T, Shioda A, et al. A dual computed tomography linear accelerator unit for stereotactic radiation therapy: a new approach without cranially fixated stereotactic frames. Int J Radiat Oncol Biol Phys. 1996;35:587-592.
- Onishi H, Kuriyama K, Komiyama T, et al. A new irradiation system for lung cancer combining linear accelerator, computed tomography, patient self-breath-holding, and patient-directed beam-control without respiratory monitoring devices. Int J Radiat Oncol Biol Phys. 2003;56:14-20.
- Wong JR, Cheng CW, Grimm L, Uematsu M. Clinical implementation of the world?s first PRIMATOM, a combination of CT scanner and linear accelerator, for precise tumor targeting and treatment. Phys Med. 2001;17:271-276.
- Sidhu K, Ford EC, Spirou S, et al. Optimization of conformal thoracic radiotherapy using cone-beam CT imaging for treatment verification. Int J Radiat Oncol Biol Phys. 2003;55:757-767.
- Ford EC, Chang J, Mueller K, et al. Cone-beam CT with megavolage beams and an amorphous silicon electronic portal imaging device: potential for verification of radiotherapy of lung cancer. Med Phys. 2002;29:2913-2924.
- Jaffray DA, Siewerdsen JH, Wong JW, Martinez AA. Flat-panel cone-beam computed tomography for image-guided radiation therapy. Int J Radiat Oncol Biol Phys. 2002;53:1337-1349.