Running the Numbers
In the Zone: Molecular Imaging at RSNA
The Long and Short of Inverse Planning
Ebb and Flow
Product Showcase: Real-Time Target Tracker Now Available for IMRT, IGRT, and SRS
DVD Series Reviews Treatment and Management of Prostate Cancer
ACRIN RFA Trial Still Enrolling Sites
UB Receives Grant to Develop Hybrid Imaging Techniques
Product Showcase: Clinical Oncology Management Environment Created for Dynamic Adaptive Radiotherapy
Running the Numbers
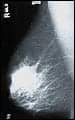
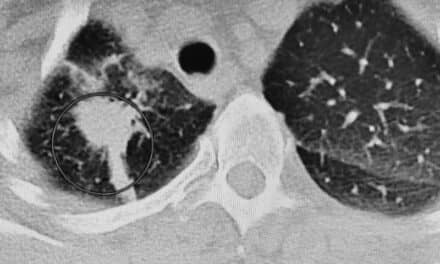
2 additional years was how long lung-cancer patients who underwent chemotherapy and radiation after surgery lived than those patients who had only chemotherapy after surgery. The study1—part of a larger randomized study called ANITA 1—examined 840 patients with non?small-cell lung cancer that had spread to the mediastinal lymph nodes. Radiation was not randomized nor mandatory, but only recommended for these patients; 232 received adjuvant radiation at doses ranging from 45 to 60 Gy, 2 Gy/fraction, five fractions per week using a high-energy linear accelerator. Researchers found that additional radiation after chemotherapy benefited those patients whose cancer had spread to the mediastinal lymph nodes. At that stage, those who underwent chemotherapy and radiation after surgery lived almost 2 years longer (47 versus 24 months) than those patients who had only chemotherapy after surgery.
“This is the first time that a clinical trial has examined the effectiveness of radiation after surgery for lung cancer,” Jean-Yves Douillard, MD, PhD, lead author of the study and a medical oncologist at the Centre Rene Gauducheau, St Herblain, France, said in a press release. “The results show that radiation treatment should be considered for resected non?small-cell lung cancer with involved mediastinal lymph nodes in addition to chemotherapy. The data observed in this study, however, needs to be confirmed in a prospective randomized trial of radiation in addition to chemotherapy.”
Reference
- Douillard J, Rosell R, De Lena M, Riggi M, Hurteloup P, Mahe M. Impact of radiation on survival after complete resection of non?small-cell lung cancer: Descriptive analysis in the randomized adjuvant chemotherapy trial, ANITA 1. Int J Radiat Oncol Biol Phys. 2006;66(3)(suppl 1):S2.
In the Zone: Molecular Imaging at RSNA
By Cat Vasko
At RSNA 2006, advancements in molecular imaging were highlighted via inclusion in the “Molecular Imaging Zone.” Here, Medical Imaging looks at some of the technology featured in the zone, from fusing software to 64-slice PET/CT.
Dedicated Cardiac PET/CT and SPECT/CT
GE Healthcare, Waukesha, Wis, debuted its newest dedicated software for SPECT/CT and PET/CT, the CardIQ Fusion package. As its name suggests, CardIQ Fusion brings together anatomical and physiological data from CT, PET, and SPECT images, allowing multimodality analysis within a single application. CardIQ Fusion has been under evaluation at hospitals worldwide, including University Hospital, Zurich; and at both Brigham & Women’s Hospital, Boston, and Vanderbilt University, Nashville, Tenn. An image generated using the platform received the “Image of the Year” award from the Society of Nuclear Medicine (SNM) in 2006.
CardIQ Fusion merges anatomical data, such as coronary angiography, with physiological data, such as perfusion or viability, enabling more detailed visualization of cardiovascular disease. Images can be viewed in a 3D volume-rendered format or in 2D reformats, such as axial, sagittal, coronal, and curvilinear views, and anatomical and physiological data registers simultaneously. The correlation between the anatomical and physiological, such as the stenotic coronary artery and the relevant myocardial radiotracer uptake distribution, then can be used to identify the vessels in question and determine the proper treatment method. Images generated for the same patient but on different systems and on different dates also can be fused together for analysis.
Laser Mammography Technology
New to the Molecular Imaging Zone was Imaging Diagnostic Systems Inc (IDSI), Ft Lauderdale, Fla, displaying its CT laser mammography (CTLM) technology, intended for use as an adjunct to mammography. Currently, IDSI is seeking premarket approval for the CTLM system; the FDA has determined that the company’s clinical investigation is a nonsignificant risk investigational device study. CTLM enables 3D breast imaging via visualization of tumor angiogenesis. During CTLM imaging, the breast hangs in its natural position and is scanned without ionizing radiation for 10 to 15 minutes; CTLM also penetrates dense tissue and implants more easily than conventional mammography.
64-Slice PET/CT and SPECT/CT

|
| The Precedence system from Philips Medical now provides 64-slice CT fused with PET or SPECT. |
Philips Medical Systems, Andover, Mass, has merged its 64-slice CT technology with both PET and SPECT platforms for faster, higher-resolution molecular imaging. The Precedence SPECT/CT system can produce CT-based attenuation correction, image myocardial perfusion imaging in half the time of conventional scanners, and perform advanced cardiac CT procedures like calcium scoring and coronary CTA in one scan. Precedence also boasts a high level of flexibility, offering SPECT/CT, CT-only, or SPECT-only studies.
The Gemini TruFlight PET/CT system offers 16-slice or 64-channel PET/CT featuring time-of-flight PET imaging. The time-of-flight functionality more precisely localizes the PET annihilation event, shortening scan time and lowering dosage. The system’s low count rate results in improved image quality, making it ideal for imaging larger patients; and the 64-channel configuration enables faster, more precise coronary CT angiography.
Low-Dose Cardiac Imaging
Spectrum Dynamics Inc, Danville, Calif, announced FDA 510(k) clearance of its D-SPECT cardiac imaging system, which uses proprietary BroadView technology for functional perfusion imaging. D-SPECT distinguishes itself with a unique gamma camera that uses tungsten collimators and 9 small, solid-state cadmium zinc telluride (CZT) digital detectors. The CZT enables photon collection from hundreds to thousands of different angles, resulting in shorter acquisition time and the potential to reduce dosage without compromising image quality.
The D-SPECT cardiac scanner also increases patient comfort by using a chair-based upright platform. Patient data is encrypted onto an “RScan” radiotracer syringe and wristband, and the D-SPECT system automatically detects and reads this data, optimizing workflow and throughput. In 2008, Spectrum Dynamics hopes to introduce a hybrid D-SPECT/CT system to combine functional and anatomical imaging.
Cat Vasko is associate editor of Medical Imaging. For more information, contact .
The Long and Short of Inverse Planning
The Georgia Institute of Technology?s advanced algorithms allow clinicians to plan brachytherapy treatments in less time and with greater accuracy than conventional methods
By Renee DiIulio
The term “brachytherapy” stems from two Greek words: brachys, meaning short, and therapeia, meaning therapy. “Short” refers to the intended distance between the radioactive seeds and the tumor they are designed to eradicate. Until now, short has in no way referred to time, either for planning the treatment or implanting the seeds. However, researchers at the Georgia Institute of Technology, Atlanta, have created advanced algorithms that have changed all that.
Licensed to Prowess Inc, Chico, Calif, the advanced mathematics have been incorporated into the company’s Panther Brachy InversePlan system, released in December for clinical use nationwide. The new methodology allows the creation of a brachytherapy plan within 1 minute as well as real-time optimization during the seed-implantation procedure.
Unlike forward planning—where the clinician places the radioactive seeds using a computer model, checks the dose, and then modifies placement until the dose on-screen matches the desired properties—inverse planning starts with the clinician’s constraints, which the computer then uses to devise a plan.

|
| Eva Lee, PhD. |
The mixed-integer algorithms and software remove much of the guesswork; currently, clinicians can spend 2 to 4 hours creating a forward plan. “Most physicians do not have this amount of time to devote to one plan,” says Eva Lee, PhD, associate professor and director of the Center for Operations Research in Medicine at the School of Industrial Systems and Engineering, Georgia Institute of Technology.
The new algorithms incorporate a large number of factors, such as the dose of each radioactive seed, the shape of the organ being treated, the location of tumor cells within the organ, the location of critical structures for which the radiation dose should be limited, the sensitivity of tissues to radiation, and the expected shrinkage of the organ after treatment. The clinician establishes these criteria, enters the data into the program, and is able to view the implantation plan on-screen in as little as 20 seconds.
Because of the length of time required to complete a forward plan, patients must come in twice: once for the imaging that will be used in planning, and a second time to have the plan executed. The time between the two visits can be problematic—tumors can change, and the devised plan could be outdated by the time the patient comes in for treatment. The outmoded plan can negatively impact tumor coverage and normal tissue complications.
The immediateness of inverse planning avoids these problems. Lee notes that studies have shown the methodology to offer 100% tumor coverage. “In prostate cancer patients, we have seen the prescription dose contour tight to the prostate while the dose to the urethra and rectum has been reduced by 20%,” she says.
Being able to image and calculate in real time also means that complications can be handled with a better outcome. Often, physicians encounter difficulties placing seeds due to blockages in the needle path. Forward planning would require the physician to make ad hoc modifications; inverse planning allows a new plan to be reconfigured quickly.
But the ability to quickly optimize a plan offers benefits beyond better outcomes and less time at the drawing board. Patient comfort and procedure cost also are positively impacted. “The program develops the best seed configuration and displays positioning on the screen along with information about which needle to use,” Lee explains.
The information has led to a reduction of roughly 15% to 20% in the number of seeds placed using inverse planning, according to Lee. Fewer seeds result in a shorter procedure with less patient discomfort and less expense. “At $50 to $100 per seed, that is a significant cost savings,” she notes.
Prowess’ existing customers will be the first to realize these benefits. The company is currently adding the new algorithms to the approximately 700 systems in use. Although many are likely to be used in prostate cancer treatment, other oncological diseases can benefit as well. “Prostate cancer has a lot of visibility, but breast cancer research is catching up. The system is really applicable to any part of the body,” Lee says. She is currently collaborating with other researchers to improve treatments for breast, lung, cervical, brain, and liver cancers. And she doesn’t have such a long way to go.
Renee DiIulio is a contributing writer for Medical Imaging. For more information, contact .
Ebb and Flow
Using MR systems to quantify the efficacy of new pharmaceuticals
By Dana Hinesly
The powerful imaging technology available today is not only helping patients, but also providing a valuable look inside the human body for pharmaceutical, biotechnology, and medical device industries seeking better remedies for what ails us. VirtualScopics works with these companies, using dynamic contrast-enhanced MRI (DCE-MRI) data to provide a method to directly measure blood flow and vessel permeability in tumors. The company recently received a patent on its method for calculating the arterial input function in DCE-MRI. Medical Imaging discussed the details of employing medical imaging in clinical trials with Edward A. Ashton, PhD, VirtualScopics’ chief scientific officer.

|
| Edward A. Ashton, PhD, VirtualScopics |
MI: What is involved with orchestrating a clinical trial using DCE-MRI?
Ashton: If the intention is to demonstrate the efficacy of a drug that is either antiangiogenic or vascular disruptive in nature, it’s very important in the early stages to measure blood flow and vascular permeability in vivo. The first step is to develop an image-acquisition protocol that is going to meet the needs of your study. In particular, you need to know whether you are interested in, for instance, changes in flow specifically, or whether you can look at a composite parameter that measures the flow and permeability together.
Once you have that in place, you need to actually go to the imaging sites where you are going to acquire the data and train them on how to run the protocol. Typically, that involves having someone at the site teach the technologists, and potentially the radiologists, exactly how to run the protocol. It could even require programming the protocol into the scanner for them and doing some test runs. We have phantoms we typically use to test the effectiveness of the protocol on each scanner we are using for a particular study. Once you have qualified the site, it can be approved to begin recruiting and scanning patients.
MI: With studies taking place in multiple locations, how do you monitor the quality of the data?
Ashton: It’s very important—particularly in the early phases of the study—to monitor the quality of the data that each of the sites is producing to ensure that they are following protocol adequately, that they are recruiting the right kind of patients, and that they are acquiring the data in a careful and consistent way. We consider it an end-to-end system-integration process, where you have materials that are “input”—essentially the patient and the imaging protocol—and what results is the data. We try to produce the best data, beginning with the preparation of the patient and continuing all the way through to data transfer to the sponsor.
Everything must be taken into account: how the patient is instructed to behave in the magnet, for instance. Do we tell the patients to try to hold their breath, to breathe shallowly, or to just breathe freely while they’re in the scanner? Is the patient made comfortable? Is the needle we’re using to give the contrast injection inserted properly into the vein? Are they using the same vein each time? These are all areas where noise can be introduced, and we feel it is our responsibility to essentially quash those errors wherever they show up.
MI: How do you ensure those errors don’t find their way into the data?
Ashton: It’s the system we’ve put in place, which begins with designing a protocol, and includes a very systematic method for training the sites and qualifying the scanners at the location. A site has to pass all of these tests before they are allowed to begin acquiring data. We also have very strict quality-control procedures in place in our core lab for exactly how the analysis needs to be done. And most of the analysis is, in fact, automated and scripted through a database, so there are no opportunities for human error. And, of course, we spend a lot of time working on the modeling software itself—because, as with most complex processes, there are a lot of different ways to do the modeling, and we have worked very hard to develop a method that is as noise-free as possible.
MI: How do the drug companies translate the results of these studies into drug development?
Ashton: This sort of data typically is used for demonstrating mechanism of action. So, if a company is testing a tubulin-binding agent and believes it is going to cut off flow of blood to the tumor, DCE-MRI gives you a direct window into the anticipated effect. The sponsor can run a Phase I trial in 15 or 20 patients; if there isn’t any reduction of the blood flow to the tumors, that’s a pretty strong signal that the drug is not, in fact, having an effect at the doses being administered. Alternatively, if the images indicate that the compound is working as expected, it is a very strong signal that the company can push forward into a large Phase II program with confidence that the study will have positive results.
MI: So, it is possible for VirtualScopics to determine results with smaller sample sizes?
Ashton: Right. One of the benefits of inserting this sort of technology into the clinical-trial process is that because you are looking directly at the biological effect of the drug, you are able to make decisions about drug efficacy with much smaller patient populations than was possible before. Traditionally in a cancer study, for instance, you would wait until late Phase II—when you have survival data on a few hundred patients—to decide if the drug is having a significant effect or not. But at that point, the company has invested tens of millions of dollars into the drug already, so it becomes very painful to cut off the development process at that stage. Whereas, with systems like the ones we are putting in place, you can have that efficacy signal with a very small number of patients at a point when the investment is only a few million dollars, and it’s much easier to then cut off the development if that’s what needs to be done.
MI: Which modalities can be used for these types of studies?
Ashton: We work with a range of modalities. When measuring blood flow, there are several techniques you can use. We’ve worked with CT, but because of the substantial radiation dose it delivers, it is somewhat less popular. There is a technique called O-15 PET that can be used, which also is very useful and very well-validated. The problem with this method is that O-15 PET is relatively expensive and not widely available; for those reasons, it is also not quite as popular. There are always lots of options with imaging, and it’s important to know the advantages and drawbacks of each one so you can find the right one for your program. One of the benefits we present to the drug companies we work with is laying out several different options for obtaining the information they need—along with the advantages and disadvantages of each.
MI: And then letting them decide which method is best?
Ashton: Yes, they can weigh all the factors against one another and determine what will work best. For example, if they need to see the difference between flow and permeability, DCE-MRI would not be right for that program. Instead, they would need to go with dynamic susceptibility contrast MRI or DCE-CT, which are more easily able to look at those parameters independently.
Dana Hinesly is a contributing writer for Medical Imaging. For more information, contact .
Product Showcase: Real-Time Target Tracker Now Available for IMRT, IGRT, and SRS

|
| Initia-RT?s TrackBeam delivers real-time target tracking using the linear accelerator?s treatment beam. |
Initia-RT, Tel-Aviv, Israel, now offers the TrackBeam device, which is capable of tracking a moving target while delivering radiation treatment using collimator-based technology. TrackBeam incorporates two of the company?s other products:
- TrackLeaf cross-leaf micro multi-leaf collimator (mMLC), which offers high-resolution real-time tracking of a shaped aperture; and
- TrackPort?a mini-portal imaging device that easily attaches and is precisely registered to the mMLC?acquires real-time video images and delivers processed data to TrackLeaf for immediate response.
By integrating these two products, TrackBeam delivers real-time target tracking using the linear accelerator?s treatment beam. The device?s configuration allows for beam-steering with real-time target localization and tracking using dynamic aperture shaping. Track-Beam is optimal for intensity-modulated radiation therapy (IMRT), image-guided radiation therapy (IGRT), and stereotactic radiosurgery (SRS). Specifically with IGRT, TrackBeam takes into account internal organ motion and real-time target tracking. Visit www.initiamed.com for additional information.
DVD Series Reviews Treatment and Management of Prostate Cancer
A new three-part DVD series developed by Prostate Oncology Specialists, Marina del Rey, Calif?a medical group focusing on prostate cancer prevention and management?will review diagnosis and treatment of every phase of the disease. The DVDs offer patients and their loved ones an introduction to prostate cancer diagnosis, a look at the disease?s varying degrees of aggressiveness, and the proper method for selecting appropriate therapies. The three DVDs cover the following information:

|
| Prostate Oncology Specialists? three-part DVD lecture series for prostate cancer patients, families, and physicians. |
- A New Perspective: Look Before You Leap. This DVD contains a lecture by Mark Scholz, MD, medical director of Prostate Oncology Specialists, which examines the rapidly shifting field of prostate cancer treatment. The disease is increasingly being separated into two categories?chronic but non?life-threatening, or aggressive and life-threatening?requiring combination treatment. Scholz?s lecture here focuses on treatments for the chronic form of the disease, looking at how men can safely forgo immediate radical treatment through a monitoring process known as active surveillance. Scholz also looks at intermediate-risk prostate cancer, looking at a management method involving testosterone-inactivating pharmaceuticals (TIP) as an alternative to radical therapy.
- Systemic Treatments for Prostate Cancer?Why Are Medicines for a “Localized” Cancer Needed? In this lecture, Richard Lam, MD, director of
- clinical research at Prostate Oncology Specialists, looks at systemic metastasis, microscopic cancer outside of the prostate gland that often goes undetected by clear bone scans and CT scans. Men with microscopic metastasis generally receive little benefit from surgery only or radiation therapy only. Lam explains how to identify patients most likely to have micrometastasis and discusses potential treatments, including TIP, radiation therapy, docetaxel, immune-based compounds, targeted drugs, and experimental agents.
- Testosterone-Independent Prostate Cancer. On this DVD, Scholz explains how to spot the early signs of testosterone resistance for patients who have been controlling their prostate cancer for years via testosterone blockade; delaying therapy when the disease has become resistant decreases the effectiveness of additional treatments. Scholz also examines the potential therapies so that patients might better select the appropriate treatment.
Visit www.prostateoncology.com for copies of the DVDs or for more information.
—C. Vasko
ACRIN RFA Trial Still Enrolling Sites
The American College of Radiology Imaging Network (ACRIN), Philadelphia, opened enrollment for a data-gathering trial of radiofrequency ablation (RFA) in December 2005. One year later, ACRIN is 100 patients away from its target enrollment of 120. Site enrollment is still open, and the study is funded, although the trial “is not incentivized relative to recruitment,” according to Gerald Dodd, MD, professor and chair of the department of radiology at the University of Texas Health Science Center at San Antonio.
The trial, officially titled the “Multi-Center Feasibility Study of Percutaneous Radiofrequency Ablation of Hepatocellular Carcinoma in Cirrhotic Patients,” will evaluate RFA?s control of hepatic tumors over 18 months. “The study is designed so that all patients are followed for a year and a half after enrollment,” Dodd says. “The patients are treated, and they?re allowed to be re-treated with ablation as much as is necessary over the first 15 months following enrollment. What we?re looking for is to determine by CT what percentage of patients we can maintain disease-free at 18 months.”
But there?s been an unanticipated lag in bringing sites into the trial. “The lead sites have about six patients enrolled,” Dodd explains. “But those are the early sites. If we do, in fact, achieve 20 sites, our enrollment should accelerate substantially.” An institution is eligible for the trial if the radiologist who will perform the procedure has previously treated at least 15 liver tumors with RFA, including at least five with the Valleylab/Radionics device designated for use. The site also must have a helical CT scanner with a power injector, and must employ a pathologist to send slides to a central pathologist for review.
“I think it will be a successful trial,” Dodd says. “And, of course, the results will be very interesting.” The ACRIN 6673 protocol-specific application is available online at www.acrin.org/6673_protocol.html.
—C. Vasko
UB Receives Grant to Develop Hybrid Imaging Techniques
The Institute for Lasers, Photonics, and Biophotonics at the University at Buffalo (UB) aims to usher in the next generation of medical imaging. To support its efforts, the center has been awarded a $1.1 million grant from the John R. Oishei Foundation, Buffalo, NY. Funds from the “Developing New Advances in Medical Imaging Through Nanotechnology” grant will cover the Institute’s work with nanoparticle-based multiprobe systems over the next 3 years.
Led by Paras Prasad, PhD, executive director of the Institute and a State University of New York (SUNY) distinguished professor of chemistry, the team is developing these systems to aid in the early diagnosis of cancer and other diseases. The hybrid images are expected to provide clinicians with more comprehensive—and, therefore, more clinically useful—data than is collected from single imaging techniques. It is expected that the correlation seen between molecular and morphological changes at the cellular level will provide a more sensitive and accurate picture of disease progression, even in very early stages.
“Ultimately, clinicians want the most complete data possible that they can gather from medical images, ranging from tissue structure to metabolic processes to molecular markers. We are aiming to provide them with such data by developing nanoparticle platforms capable of carrying multiple contrast agents for complementary medical-imaging techniques in the same nano-sized package,” Prasad said in a press release.
In addition to permitting simultaneous use in different imaging modalities, the particle surfaces can be modified to carry specific agents, such as antibodies, that detect specific disease markers. The team creates the nanoparticles using organically modified silica (ORMOSIL). Current development is focused on five areas, including optical imaging; MRI using fluorine nuclear probes; PET, CT and SPECT; and ultrasound imaging:
- Optical imaging nanoparticles in development will combine fluorescent imaging with Raman imaging, a method of chemical analysis at microscopic levels, or the new modality Coherent Anti-Stokes Raman Scattering imaging. The team expects results to provide information on the early molecular indications of disease as well as cell response to specific stimuli, such as a drug.
- New probes based on fluorine-19 and developed as contrast agents will allow simultaneous MRI and PET scanning. The images will show both structural and metabolic information.
- The researchers will combine PET with optical imaging, using 124I-incorporated ORMOSIL nanoparticles as PET contrast agents. These images are expected to permit a more accurate assessment of drug efficacy.
- CT and SPECT will be paired not only with each other but also with optical imaging to create a trimodal scan showing circulatory, tissue, and cellular disease aspects. The nanoparticles will incorporate radio-opaque ions, radiolabeled Annexin (or other biotargeting agents), and fluorescent molecules.
- The group will explore the use of nanoparticles and hybrid microbubbles in ultrasound. If the work produces a contrast agent for ultrasound and a delivery vehicle for nanoparticles, the “nanocarriers-within-microcarriers” concept could permit the hybridization of ultrasound with any of the other imaging modalities being studied (optical, MRI, PET, CT, and SPECT).
Although the team states in its research grant that the ultrasound work will begin after the other modality work has been accomplished, a portion of the grant will be used to bring on a research professor with expertise in ultrasound imaging.
Additional funding has been received from UB’s New York State Center of Excellence of Bioinformatics and Life Sciences; Prasad is affiliated with the Center’s bioengineering/tissue engineering team. Research is being conducted in collaboration with Johns Hopkins Medicine, Baltimore, and Roswell Park Cancer Institute, Buffalo, NY.
Renee DiIulio is a contributing writer for Medical Imaging. For more information, contact .
Product Showcase: Clinical Oncology Management Environment Created for Dynamic Adaptive Radiotherapy
Varian Medical Systems Inc, Palo Alto, Calif, has added new capabilities to its radiotherapy information-management and treatment software, making it possible to modify plans with up-to-the-minute images generated via image-guided radiation therapy. Exhibited at the 2006 meeting of the American Society of Therapeutic Radiologists and Oncologists in November, the Inspiration clinical oncology management environment for dynamic adaptive radiotherapy now enables modification of the treatment plan at any point during a patient?s course of treatment for cancer.

|
| Using Inspiration from Varian, a therapist sits at the company?s 4D treatment console, which offers access to the ARIA information system and the Eclipse treatment-planning system, as well as controls for the On-Board Imager device, RPM respiratory gating, and the treatment-delivery system. |
“Before now, if a doctor suspected a change in the patient?s anatomy during a course of treatment, he would have had to create a new treatment plan from scratch,” Corey Zankowski, senior director of software systems marketing at Varian, said in a press release. “Now, with the connections built into the Inspiration environment, clinicians can adapt any plan in the Eclipse treatment-planning system, and all of the internal bookkeeping is managed automatically. The Inspiration environment keeps track of all such changes as well as who made and authorized them, and the treatment plan is always up-to-date, which is essential for treatment techniques that are designed to adapt to changes in the patient over time.”
The Inspiration environment, which is anchored by the ARIA oncology information system, connects multiple elements, including the Eclipse treatment-planning system, the Acuity simulator, the Clinac or Trilogy linear accelerator, and the On-Board imager device for generating images to guide radiation therapy treatments. The Millennium multi-leaf collimator and the RPM respiratory gating system also can be linked into Inspiration.
For more information, visit www.varian.com.
—C. Vasko