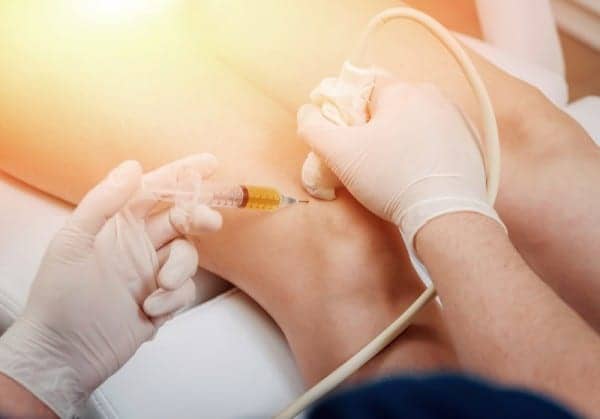
A new white paper discusses the prevalence of ultrasound-guided peripheral intravenous (UGPIV) procedures, the challenges associated with obtaining UGPIV access, and solutions for hospitals to improve patient safety while lowering costs.
Author Nancy Moureau, RN, PhD, CRNI, CPUI, VA-BC, says that given the rise in UGPIV, the information in the white paper applies not only to vascular access specialists but to any clinician performing ultrasound-guided peripheral or midline insertions in a variety of care settings. Moureau is an internationally recognized expert and consultant in vascular access, and the CEO of PICC Excellence, Hartwell, Ga.
“As a vascular access educator, I observe many clinicians using ultrasound guidance to obtain intravenous access and I’ve noticed there’s a lot variation in technique. I wanted to address the importance of maintaining a proper aseptic insertion to reduce contamination and help clinicians have a better understanding of the available options that contribute to successful and safe UGPIV procedures,” says Moureau, who is affiliated with Greenville Memorial and University Medical Center in South Carolina, as well as the Alliance for Vascular Access Teaching and Research Group (AVATAR) based in Australia.
With more than two billion peripheral IVs sold worldwide each year, PIV insertion is the most commonly performed invasive medical procedure in hospitalized patients. According to Moureau, however, more than 50% of patients are considered to have difficult vascular access, which necessitates the use of ultrasound guidance in order to successfully achieve peripheral access and administer necessary treatments.
The benefits of UGPIV include fewer failed insertion attempts and avoiding the need for more invasive central venous access devices, both of which save time and money and contribute to greater patient satisfaction. However, there is a greater risk of contamination due to extended procedure time and the presence of the ultrasound transducer and gel in the sterile puncture area, Moureau says. Infection control methods, such as sterile probe covers and single-use sterile gel packets, can limit the risk of infection, but significantly increase the cost of the procedure, she says.
“Achieving PIV access with ultrasound guidance can be very challenging. It takes more time with these challenging difficult access patients, and as the length of the procedure increases, so does the risk of contamination,” says Moureau. “With the additional supplies needed in order to maintain an aseptic procedure, which is essential to minimize patient risk, UGPIV becomes very costly. For a procedure that currently has little to no reimbursement, this can have a significant economic impact on hospitals over time.”
Among the solutions Moureau discusses in the white paper is a combination barrier and securement dressing that prevents the transducer and gel from coming into contact with the skin. This dressing enables a better aseptic insertion technique and lowers costs by eliminating the need for additional securement dressings, sterile gels, and probe covers.
“The all-in-one barrier and securement dressing makes it possible to perform a more efficient, cost-effective procedure without sacrificing patient safety,” said Moureau. “This type of technology is very important to me because it helps me do a better job, and I believe it will enable other clinicians to use ultrasound guidance to achieve successful PIV access in a way that is safer for patients overall.”
To learn more, visit PICC Excellence.