Innovation is the name of the game in single photon emission computed tomography (SPECT) studies.
Innovation is the name of the game in single photon emission computed tomography (SPECT) studies.
Today, innovation has brought multi-head detectors that produce high-quality images at a rapid pace that rival PET studies. Image fusion techniques are enhanced both as a result of GE Medical Systems’ (GEMS of Waukesha, Wis.) hybridized equipment that melds CT and SPECT, and through computer software packages that overlay cross-sectional data from different imaging modalities, as does syngo from Siemens Medical Systems Inc. (Iselin, N.J.). A totally new approach to detector configuration is offered by ADAC Laboratories Inc. (Milpitas, Calif.), as a new receptor imaging agent facilitates clinical studies that promise to improve early diagnosis of Parkinson’s disease and attention deficit hyperactivity disorder (ADHD).
 Multi-head detectors
Multi-head detectors
SPECT has evolved from a technique for obtaining cross-sectional imaging of the body using radiopharmaceuticals with single-headed detectors, to multi-head instruments that orbit around a body or organ.
“A multidetector camera array increases throughput, so the patient doesn’t have to remain motionless as long on the table,” explains Milton Guiberteau, M.D., chief of nuclear medicine at St. Joseph Hospital (Houston) and professor of radiology
at the University of Texas (Houston). Guiberteau also serves as the chair of the American College of Radiology Nuclear Medicine Commission.
“Right now, cardiac SPECT is the No. 1 use,” he adds. Close to 40 percent of all SPECT studies involve functional imaging of the heart.
Triple-detector cameras have been around for a number of years. With one detector to obtain a three-dimensional data set, the camera must go around the patient 360 degrees. With two detectors, the exam requires a 180-degree rotation, in contrast with three detectors, which require only 120 degrees. The more detectors that are placed in an array around the patient, the more quickly the data are collected.
“The most common SPECT imaging other than heart is bone SPECT,” says Karl Kellar, product manager for nuclear oncology at Marconi Medical Systems Inc. (Highland Heights, Ohio). “For low back pain, an MRI is usually performed. When that study does not show a definitive cause, SPECT often can help with the differential diagnosis. You do a bone scan and see an abnormal region, but you cannot be sure if it’s in the spinal canal or bone. If you combine MR with SPECT, you can see precisely where the lesion is.”
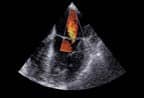
James K. O’Donnell, M.D., director of nuclear medicine at University Hospitals of Cleveland (Ohio), relates that his department performs 100 percent of its nuclear medicine cardiac studies using SPECT. A routine method for a cardiac perfusion study is to administer one injection of a radiopharmocologic agent to acquire images of a patient’s myocardium at rest and deliver another dose with the patient at peak stress on a treadmill.
“We’re looking for a defect that may be there at stress. If that area perfuses normally when the patient is at rest then we have documented ischemia that may require intervention,” O’Donnell explains. “If there is a defect at stress which also is a defect at rest, the implication is that it is an infarct that doesn’t perfuse at all.”
O’Donnell — who uses Siemens’ E.Cam — describes a new technique in which clinicians synchronize image acquisition with the electrocardiogram. With ECG gating, the heart can be viewed two different ways.
“We look at it as a perfusing muscle with stress and rest images,” says O’Donnell. “Then we look at it as a pump with ECG gating.”
Don Lien, M.D., nuclear radiologist with Dutchess Radiology Associates (Poughkeepsie, N.Y.), uses cardiac SPECT at the Columbia Memorial Hospital (Hudson, N.Y.). Because the heart is obliquely oriented in the body, standard views make it more difficult to diagnose coronary artery disease with the necessary degree of accuracy.
“Conventional planar images are difficult to evaluate because of overlying structures,” Lien says. “Because it is a volumetric acquisition, we can orient the heart in projection to allow us to visualize better.” In their clinical practice, these physicians also use SPECT for tumor localization and skeletal pathology, among other studies.
Still other clinicians are finding additional applications for SPECT.
“We are using SPECT imaging of the spine to aid in the management of back pain,” says Robert Licho, M.D., assistant professor of radiology at the University of Massachusetts Medical School (Worcester, Mass.).
“Perhaps the most useful scenario is when structural imaging demonstrates many findings, but it’s not clear which findings are relevant at the present time,” he adds. “At other times, structural imaging studies are negative and SPECT will often find an abnormality that structural imaging studies do not.”
For example, if a patient has a history of refractory lower back pain and CT, MRI or X-rays show multiple abnormalities, the treating physician needs to know which abnormalities are active foci causing symptoms. Bone SPECT studies generally show increased uptake only in the active, pain-producing areas, which can direct therapy both for minimally invasive treatment, such as steroid/lidocaine injection, as well as surgery.
“My sense is that the back pain specialist will try to do the least invasive procedure possible at any given time, to preserve options down the road,” Licho continues. “I believe bone SPECT helps to target the location of intervention, maximizing the benefit of each incrementally invasive procedure when needed.”
Image fusion techniques
Because SPECT imaging provides functional or physiologic data, it serves as a valuable adjunct to imaging modalities that offer anatomical views. GEMS has developed a hybrid imaging modality that brings two powerful technologies together. The Hawkeye imaging system combines functional or physiologic imaging data from SPECT with anatomical information from a CT scan.
“We have taken a dual-head SPECT camera that can perform SPECT and FDG imaging and applied a CT tube and detector to that slip-ring gantry,” explains Beth Klein, GEMS’ global general manager of nuclear medicine and PET.
 Marconi’s Irix nuclear
Marconi’s Irix nuclear
medicine gamma camera
Hawkeye has received FDA 510(k) marketing clearance and is being used at five sites. To date, clinicians have used the Hawkeye system to complete more than 500 patient studies.
“It provides clarity, accuracy and confidence to the diagnoses and provides better methodology for attenuation correction,” Klein adds.
In the 500-plus studies, the management of a patient’s condition has changed in 20 to 25 percent of those cases as a result of what physicians viewed in a Hawkeye image. For example, when a tumor is detected in a patient’s chest wall, the clinician may not be sure of the exact location. Is it the skin, muscle layers, sternum or lung tissue? Because the Hawkeye system precisely locates the tumor, appropriate treatment measures are clarified.
“This is a very low-dose CT tube, about 1/100th of a typical CT exam,” explains Allen L. Smith, Ph.D., operations manager for GEMS’ nuclear/PET business. “It is about the exposure rate of bone densitometry. It uses a 2.5 milliamp tube that we would traditionally use in dentistry.”
Vanderbilt University Medical Center (Nashville) was involved with the development of Hawkeye and has conducted more than 100 clinical studies to date. The Hawkeye is affixed to GEMS’ Millineum VG system at a cost of approximately $800,000. Customers have the option of beginning with the VG system and upgrading to a full Hawkeye at a later date.
“Most physicians are more comfortable with anatomy than physiology,” says Martin Sandler, M.D., Vanderbilt’s chairman of radiology and radiological sciences. “They need to know that if it is abnormal, where is it abnormal. The ability to provide this information enhances the diagnostic efficacy of nuclear medicine.”
Sometimes, image fusion is accomplished with computer software that overlays information from SPECT with a CT or MRI scan.
With syngo, Siemens adopts a common computer operating system and architecture for all of the various imaging modalities. Syngo instantaneously takes the information and can compare nuclear medicine, MRI and CT images. Syngo — the common software for all modalities — provides a level of connectivity designed to improve the correlation of imaging data.
“When a tumor invades the lymph nodes, it becomes metabolically active a long time before it gets big enough to be noticed on CT as abnormal,” says University Hospital of Cleveland’s O’Donnell. “We find hot spots that correspond to tumors that develop later. Bringing anatomy and physiology back together with these fusion techniques is very promising.”
Outside the box
ADAC Laboratories in April received FDA 510(k) clearance for its new Skylight open gantry SPECT camera. In most SPECT systems, detectors are mounted in a gantry array around the patient’s body. Skylight is configured as an open camera design suspended from arms in the ceiling and the walls.
 |
 |
| Nuclear medicine image of a brain with stage 2 Parkinson’s disease (left), and without Parkinson’s disease (right), courtesy of the University of Massachusetts Medical School. | |
“Basically, the patient steps into a room and the cameras come from above, from the side, from all angles,” explains Jody Garrard, ADAC’s segment manager of general nuclear medicine, ADAC Laboratories.
The technologists and physicians also gain better access to the patient during an exam. Some patients who require imaging may have IVs or other lines that require attention, while other imaging studies may require injections during the course of the study. Sometimes, a physician needs to mark a patient’s body to indicate where surgical incisions will be made.
To ease clinician comfort with this new system, ADAC has designed software to operate the cameras in either gantry mode or free-dimensional mode. Using the software, a clinician can operate in gantry mode with no need to provide direction for individual camera motion to obtain the study.
“There is a growing interest in medicine for hybrid surgical suites,” explains Garrard. “A Skylight system could be installed in an operating room. Before you close the patient, you could image them again to determine if you got all of the lesion.”
ADAC expects Skylight to become commercially available by the middle of next year.
Advances in imaging agents
There are dozens of new imaging agents being developed, including receptor imaging agents that attach to very specific sites or substances. Altropane, under development by Boston Life Sciences Inc. (Boston), is a radiopharmaceutical imaging agent that binds with dopamine transporters (DATs). The agent currently is being evaluated in stage three multicenter clinical trials as a specific detector for Parkinson’s disease.
“In the 21st century, there will be intense research and possibly progress in neuro-regeneration,” explains Bertha K. Madras, Ph.D., professor of psychobiology in the department of psychiatry at Harvard University, School of Medicine (Cambridge, Mass.). We know that at the time Parkinson’s disease is diagnosed, at least 50 percent of the neurons are already dead, and some investigators place it at 80 percent. The real challenge is if these neuroregenerative/restorative approaches are to work, you must catch the disease at an earlier stage.” This imaging agent has shown sensitivity to detect neuron loss as low as 30 percent.
“The goal in phase III, which recently completed accrual, is to test I-123 Altropane in its ability to distinguish between Parkinsonian syndromes, including Parkinson’s disease (PD), and non-Parkinsonian syndromes,” says Licho. “Altropane is designed to be specific for Parkinsonian syndromes. It may become the first FDA-approved neuroimaging study that specifically looks at movement disorders.”
The University of Massachusetts Medical School is one of the sites participating in the multicenter trial. Licho’s department used a Marconi triple detector fanbeam SPECT camera in performing their clinical evaluation of Altropane.
“My sense is that Altropane is as sensitive for PD, if not more so, than fluoro-dopa (FDOPA) PET scanning. On a high-resolution, triple-detector camera, SPECT images are nearly as detailed as FDOPA-PET images” notes Licho. “Specificity amongst the Parkinsonian syndromes is being evaluated, but also seems comparable to FDOPA PET. An Altropane SPECT study won’t require such an elaborate medical imaging center such as a PET lab, requiring only high-resolution SPECT equipment. SPECT imaging has the advantage of being less complicated than PET and having lower internal and external cost.”
Another proposed diagnostic use for Altropane is as an objective, biologic test for ADHD. Harvard’s Madras is concerned that children are misdiagnosed in both directions — children with ADHD are missed and children who do not have the disorder are diagnosed as having it.
Altropane looks promising as a possible method of detecting ADHD on a biologic basis. In one very small study, adults with ADHD had a 70 percent higher level of dopamine transporter on average than age matched controls. Further study is necessary to confirm this finding.
“If confirmed, this could constitute, along with clinical evaluation, a straightforward and objective diagnosis of ADHD,” says Madras. Madras and her group have applied for a National Institutes of Health grant to accomplish this study.
Conclusion
The nuclear medicine market is robust and growing rapidly. New developments that improve the capabilities of gamma cameras enhance images and permit faster throughput for patient examinations. Manufacturers have focused their efforts on innovating product design, improving equipment function, and responding to the needs of nuclear medicine clinicians. In this era of cost consciousness in healthcare, improved SPECT imaging is beginning to provide data formerly only available through a PET scan. Many advances are still very much in development, but offer promise for future new applications for SPECT. ![]()