New CT technology outperforms conventional CT in detecting subtle damage in the lungs of patients with persistent symptoms of COVID-19, according to a new study published in Radiology, a journal of the Radiological Society of North America (RSNA). The technology could lead the way to earlier treatment and better outcomes for the growing number of people with COVID-19 lung damage, researchers say.
Photon-counting detector (PCD) CT has emerged in the last decade as a promising imaging tool. It works by converting X-ray photons directly into an electrical signal. This avoids the intermediate step of conversion by means of a photodiode found in conventional CT scanners that use energy-integrating detectors. The result significantly reduces energy and signal loss at the detector site. While PCD CT is not yet widely available, it has shown promise in the research setting.
“Previous studies have highlighted the advantages of PCD CT in other fields of radiology, such as cardiovascular and head-and-neck imaging, delivered by ultra-high resolution, improved image quality and, subsequently, higher diagnostic confidence of the reader,” said study senior author Benedikt Heidinger, MD, from the Department of Biomedical Imaging and Image-guided Therapy at the Medical University of Vienna in Vienna, Austria.
Dr. Heidinger and colleagues studied PCD CT’s potential as a method for imaging the lungs of people with persistent symptoms after COVID-19. They compared PCD CT with conventional CT in 20 adults, mean age 54 years. The participants had one or more COVID-19-related persisting symptoms, such as cough and fatigue.
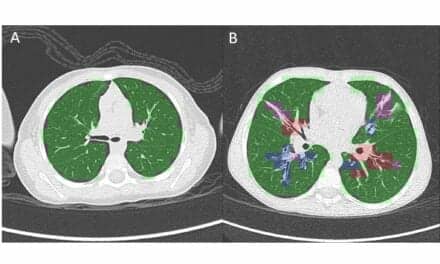
Conventional CT showed post-COVID-19 lung abnormalities in 15 of 20 (75%) participants. PCD CT revealed additional lung abnormalities in half of the participants. The most common abnormality found by PCD CT was bronchiolectasis, damage to the airways that can cause difficulties in clearing mucus from the lungs.
“In our study investigating lung abnormalities in symptomatic post-COVID patients, we were able to detect subtle lung abnormalities in 10 of 20 participants using PCD CT that were not seen in conventional CT,” Dr. Heidinger said. “Moreover, PCD CT has potential in decreasing radiation dose and in artifact reduction, representing direct benefits to patients.”
PCD CT’s ability to detect these subtle lung abnormalities is especially important, Dr. Heidinger said, because patients with persistent symptoms following COVID-19 can develop irreversible lung damage known as lung fibrosis. Conventional CT is one of the primary methods for detecting and diagnosing lung fibrosis, but it can miss the subtle abnormalities indicative of early-stage fibrosis.
“PCD CT may help to identify earlier and more effectively post-COVID patients at risk for developing lung fibrosis, and, hopefully, allow for timely treatment allocation, such as pulmonary rehabilitation, in the future,” Dr. Heidinger said.
The more accurate estimation of the severity of lung abnormalities afforded by PCD CT could also benefit lung disease monitoring and treatment response evaluation.
“Future trials including clinical outcomes such as quality of life, pulmonary function testing and histology will reveal the true benefit of this exciting new detector technology,” Dr. Heidinger said.