Neuroradiologists are very technologically savvy, and because we are not technology-phobic, we are inclined to adopt new technologies and techniques more quickly than other subspecialties. One prime example is 3D imaging, which we, at Johns Hopkins, implemented in 1991. Today, we perform 2,400 image-guided procedures every year and 3D imaging is playing an ever-growing role in many of our vascular and spinal interventional procedures, including aneurysm interventions, carotid revascularization, and acute stroke intervention.
Compared with 2D imaging, 3D offers countless diagnostic and perceptual benefits. The increased safety that information from three-dimensional imaging brings to the procedures I perform is what first motivated me to adopt the technology. I am able to see much more than before, and that has allowed me to better understand what I am treating, and ultimately deliver better care to my patients. To understand that someone has a lesion is one thing—to know the precise size, shape, and location of that lesion has improved my ability to render an accurate diagnosis and deliver the best treatment.
Procedures that require the use of 3D imaging are handled in our three biplane angiography suites or one of several CT fluoro units, which are equipped with the latest imaging technologies. Our angiography suite currently features a digital biplane fluoroscopy scanner for neuro-interventional procedures, and three older generation biplane rooms. We also have several multislice CT scanners, including 6-, 16-, and 64-slice systems for minimally invasive fluoroscopy procedures performed in the CT suite.
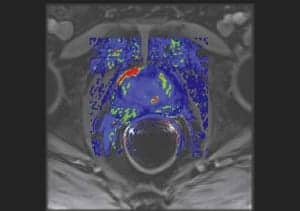
 3D fusion digital subtraction angiography of a patient with a large cervical spinal hemangioblastoma and von Hippel Lindau disease imaged using an angiography system with the ability to perform rotation 3D catheter angiography and 3D bone fusion technique. Mask acquisition enables separate display of vessels (a) or bone (b) or combined (c) in 3D. These angiographic CT-like images can resolve smaller detail than conventional 3DCT. 3D fusion digital subtraction angiography of a patient with a large cervical spinal hemangioblastoma and von Hippel Lindau disease imaged using an angiography system with the ability to perform rotation 3D catheter angiography and 3D bone fusion technique. Mask acquisition enables separate display of vessels (a) or bone (b) or combined (c) in 3D. These angiographic CT-like images can resolve smaller detail than conventional 3DCT. |
REVIEWING 3D IMAGES
Images captured in either the CT or angiography suites are sent directly to our 3D workstation for manipulation and evaluation. After selecting the desired image and patient study, I then crop, window, and level each image to minimize unnecessary soft tissue—a process that requires about 2 to 3 minutes. Following this, I proceed to review each carotid artery at the bifurcation, and look at each vessel from the arch up. I then move on to the vertebral artery—studying in particular its origin and course through the vertebrae—and determine if there is a cervical rib or aberrant insertion of a vertebral artery. I follow the vertebral artery through the jaw and skull base to the basilar artery. I repeat this process for the carotids in the head—looking for the posterior and anterior communicating arteries and the presence of intercranial disease.
NEW APPROACHES
In vascular, both CT and catheter-based angiography have become increasingly important in the evaluation of aneurysms in the brain. However, the greatest benefits are realized with catheter angiography, which images the blood vessels of the brain to detect abnormalities, such as stenosis or occlusion. 3D imaging has enabled us to better process this data and obtain CT-like images using catheter angiography technology.
This Open CT™, as I refer to it, is very useful in acute vascular and spinal interventions for interventional neurologists. In addition, Open CT may serve as a powerful hybrid tool for trauma patients that require vertebroplasty, which uses imaging equipment to repair broken vertebra with bone cement to stabilize the spine and relieve pain. In either respect, I believe Open CT will be the great new field of the future.
ESTIMATING STENOSIS
Noninvasive imaging is a wonderful tool and a great patient advocacy step. However, we must not forget that noninvasive imaging can overestimate stenosis. Ultrasound, for instance, can overestimate stenosis by as much as 15%. We, as a group, need to consider seriously the risk of overestimating stenosis when it results in patients undergoing unnecessary carotid endarterectomy that can place them at a far greater risk of stroke when compared to catheter angiography. The risk of catheter angiography causing a stroke is around or less than 1%, according to an article in the American Journal of Neuroradiology.1 The risk of carotid endarterectomy causing a stroke is at least 5% to 8%, a difference we as a group need to consider when performing noninvasive studies that guide treatment.
It also is important to keep in mind that scientific data state clearly that unless male patients are more than 70% stenotic and have at least a 5-year life expectancy, they do not benefit from carotid endarterectomy in symptomatic disease. For asymptomatic male patients, stenosis must exceed 80% to provide benefit, and again, they must have a life expectancy greater than 5 years. Studies show that there is virtually no benefit from carotid intervention to women that are asymptomatic.
 3D fusion digital subtraction angiography of a patient with a coiled intracranial aneurysm imaged with rotation 3D catheter angiography and 3D bone fusion technique, which enables visualization of the coils (a), or the vessels (b), or both (c) as a fused volume. 3D fusion digital subtraction angiography of a patient with a coiled intracranial aneurysm imaged with rotation 3D catheter angiography and 3D bone fusion technique, which enables visualization of the coils (a), or the vessels (b), or both (c) as a fused volume. |
IMPROVING PATIENT COMFORT
One significant benefit of 3D imaging is that it provides the ability to conduct procedures I was unable to do previously for patients with pain resulting from metastatic disease. Procedures of this nature, including vertebroplasty, are conducted using a combination of CT fluoroscopy, a portable C-arm, and a specially designed table on our 16-slice CT system. Under CT fluoroscopic guidance, the system allows me to safely inject liquid bone cement to solidify a pathologic fracture resulting from an underlying destruction of the bone.
Perhaps one of the most powerful, yet unexpected, benefits of 3D imaging is the role it plays in gaining informed consent from patients. 3D imaging has allowed me to bring a patient to the workstation and say, “This is what you have, this is how big it is, and this is why we need to fix it.” When we are able to present patients with images that they can truly understand, it helps translate medical science and improves patient understanding. In this capacity, axial images do not do it for patients—they need to see a 3D volume. Even if we know as physicians that a 3D volume will lose some information, it enormously helps patients grasp the significance of things.
WHAT IS NEXT FOR 3D?
Unfortunately, the adoption of 3D imaging by the medical community has been slow. I believe that there has been a massive underutilization of 3D imaging, which I attribute in large part to the reimbursement climate. In most cases, physicians receive $400 for looking at the actual cross-sectional images and only $50 for reading 3D images. It is unfortunate that nationally the medical community has not put more time into the use of 3D imaging. If we are going to maximize the power of these tools, we need to put more effort into getting as much as possible out of this minimally invasively acquired data. Just shipping the images to India and having a technologist read them is not good enough.
Kieran Murphy, MD, is associate professor of radiology and neurosurgery, and director of interventional neuroradiology, Johns Hopkins University, Baltimore.
References:
- Heiserman JE, Dean BL, Hodak JA, et al. Neurologic complications of cerebral angiography. Am J Neuroradiol. 1994;8:1401-1407.