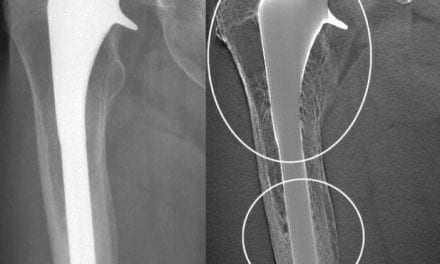
Dose reduction strategies for use of CR/DR in pediatric patients aim for the right balance of diagnostic quality and radiation exposure.
Children are not mini-adults. In addition to being smaller, children’s hearts beat faster, their respiratory rates are higher, their attention spans are shorter, and, perhaps most important for radiology professionals, their sensitivity to radiation is roughly an order of magnitude more than that of middle-aged adults.1

This seems common sense, but until more evidence was amassed regarding radiation, it wasn’t a large concern, in part because there wasn’t much to be done anyway. But advanced technologies have changed that, and awareness campaigns have advertised the problems and possibilities.
The problem is that greater sensitivity to radiation exposure, particularly combined with overexposure, is thought to increase the risk of negative consequences. In addition, early-age exposure leaves a patient with many more years during which to develop radiation-induced cancer than an older patient has, simply because of time. Though evidence proving a link between radiation exposure and cancer is still inconclusive, the association is generally accepted and has been among pediatric specialists for some time.
As a result, the radiology field has gotten much smarter about dose reduction, and facilities are successfully implementing protocols, techniques, and technologies to minimize dose and maximize quality—across all modalities, from CT to CR. As awareness of the risks of radiation exposure has expanded throughout the medical community, tips on dose reduction continue to spread as well.
Common Problems

Arl Van Moore, Jr, MD, FACR, FSIR, FAHA
Though the amount of radiation delivered during DR is much less than that during CT or film screen, children are still at risk for overexposure; CR uses a higher dose than DR but, pending anatomy to be scanned, may use higher or lower doses of radiation than plain film. In some cases, higher doses of radiation may be delivered due to necessary repeat exposure, such as when series are taken for scoliosis, or unnecessary exposure resulting from repeating inadequate scans. The use of CR and DR, in general, has increased over the past few years for many facilities—film screen has become a rare commodity in larger institutions—and only now are some radiology departments seeing their CR/DR volume plateau.
Fewer exams won’t solve the problem alone, however. Children run a higher risk of overexposure during CR, in part because of repeat exams, but also due to physiology, nervous technicians, and dose creep. Squirmy children and underexposures often mean a repeat examination, which increases the exposure of the patient. Knowing this, nervous technicians have a tendency to estimate dose too high to be sure they capture a diagnostically valuable image the first time. Because an overexposed radiographic image shows no flaws, but rather appears sharp and crisp, the overexposure can go unnoticed. Over time, the technologist unknowingly increases the exam exposure incrementally in a phenomenon known as dose or exposure creep.
Raising awareness can help, whether directed to technologists, radiologists, or ordering physicians. Referring physicians can be educated on appropriateness criteria for selecting radiology exams. Radiologists can be trained to accept more noise. And technologists should be exposed to proper pediatric technique.
“It’s a matter of providing the protocols for imaging, and then you can spend 1 or 2 hours teaching pediatric positioning techniques and refreshing people’s minds from when they were technology students,” said Lee Ball, MD, a pediatric radiologist at Providence St Vincent, Portland, Ore.
To help technologists get past their intimidation and concern regarding children, Ball also recommends using child-life specialists who can discuss developmentally appropriate strategies for assisting children in radiology environments. “Many technologists are inexperienced with children and are intimidated by them. Their concern about the kids or their fear makes it difficult for them to attend to all the other necessary technical details. And that’s probably the single greatest cause for repeat imaging,” Ball said.

Joane Chose, RT (R), takes an x-ray exam of a pediatric patient using a DR 9000 system. MeritCare Health System of Fargo, ND, has installed DR systems at several outpatient clinics to provide immediate high-resolution images for specialists and to reduce radiation dose for pediatric patients.
Size Up the Situation, Patient
Dose reduction education and methods begin with the first step in the process—the exam order. “I think, number one, you need to make sure that the examination is needed, and that it’s appropriate to be done,” said Arl Van Moore, Jr, MD, FACR, FSIR, FAHA, a radiologist with Charlotte Radiology, PA, in North Carolina, citing the American College of Radiology’s appropriateness criteria as an excellent guideline to follow.
The ultimate goal is to use the lowest dose possible to acquire an image of diagnostic quality. The choice of protocol will impact this effort. “The outcomes of the protocols do differ,” Ball said. Some options can lead to a greater dose than others.
A primary method for dose minimization is to base the level of exposure on the size of the patient rather than the age. “So if you have a young patient who weighs 100 pounds and you have an older patient who weighs only 50 pounds, the amount of dose to image the older patient would be less in general, because there’s less soft tissue to penetrate,” Van Moore said.
Many radiology departments have, therefore, created protocols specific to size and anatomy. “Our technique charts are all size appropriate,” said Brent Colby, a physicist at MeritCare Health System in Fargo, ND.
Size-based protocols also take into account the number of images required to capture the necessary information, considering anatomy and size. “Obviously, a 450-gram baby doesn’t need a separate chest and abdomen, but a 9-year-old child, who is 5 feet tall—and there are those—may need that,” Ball said.
Ball also suggests that size considerations should be factored into dose delivery across the board, but at a minimum up to the age of 18, “and maybe even a little bit older than that,” she said.
Software Solutions and More
Software can help to make protocol selection and implementation easy. Many vendors do offer low-dose optimization. “Two or 3 years ago, we got low-exposure optimization from Carestream Health Inc, Rochester, NY, and that let us drop our doses a bit more,” Colby said. Radiologist input has been key as well.
“We work with physicians constantly to find out what their tolerance for noise is. We take them to just about where they start to make noise themselves about the image quality and then we back off a little bit,” Colby said.
MeritCare also uses hardware solutions to reduce dose, such as nonstandard filtration and a reduction in exposure index. Copper filtration units have been inserted into the collimators on nearly all of the facility’s pediatric systems to absorb more low-energy photons. And the exposure index—which is really a measure of how much dose gets to the detector, Colby says—has been cut to 500 on average, and sometimes even 600, a quarter of the original dose, according to Colby.

MeritCare Health System radiologist Jacob Goldenberg, MD, reviews pediatric images captured using a DR 9000 system at an outpatient center that provides offices and imaging services for a variety of specialists.
“That’s all come as we’ve understood the technology better,” Colby said. He believes dose can be reduced even further with a switch from CR to DR, which is planned in the NICU, where the hospital’s tiniest patients are found.
“We’re using CR in the NICU, and we’re not unhappy with that, but I think we can reduce our doses and potentially bump our image quality up at the same time by moving to the DRX,” Colby said.
MeritCare has also implemented DR systems in its pediatric units, to both lower dose and decrease acquisition time. “When you’re imaging children, you sometimes have to immobilize them, so [a shorter acquisition time] decreases the time you may need to hold them in position, it decreases anxiety for the parents because the exam is done much faster, and we do see a decrease in our repeat rate when moving to that technology,” said Cathy Holmen, RTR, radiology manager at MeritCare.
In addition to dose optimization software, vendors may also offer pediatric-specific solutions. Siemens Medical Solutions USA Inc, Malvern, Pa, offers an exceptionally low table height for easier pediatric imaging with its DR system, the Ysio, and a less intimidating giraffe design for its Mobilett XP Digital and Mobilett XP Hybrid mobile x-ray systems. The Precision 500D classical R&F system by GE Healthcare, Waukesha, Wis, features a special pediatric imaging mode capable of using up to 45% less dose than the standard imaging mode with virtually no impact on image quality.
MeritCare has been working with Carestream to acquire dose-improving systems, including the new DR system (the Kodak DirectView DR System) anticipated in the NICU. In addition to low-dose optimization software, the system’s U-arm is expected to improve flexibility, patient comfort, and throughput.
More advances can be expected. As awareness increases among referring physicians and patient families, low-dose techniques may become a marketing advantage. In some areas, particularly those with high competition, they may already be a plus. Holmen notes that one physician who works with abused children refers them to MeritCare because of their dose-reduction efforts.
Marketing advantage or no, dose reduction is the “right thing to do.” Many facilities consider it a moving target that can be improved as technology advances and users become more comfortable so that dose remains strong enough for a diagnosis, but safe enough for children.
Renee Diiulio is a contributing writer for Axis Imaging News.
Reference
- Willis CE and Slovis TL. The ALARA concept in pediatric CR and DR: dose reduction in pediatric radiographic exams—A White Paper Conference. Am J Roentgenol. 2005;184:373-374.