|
Ideas in Hospital-Based Imaging |
Deficit Reduction Act Curtails Purchasing
Big Deal: Hospital Orders Carestream DR Systems
ACR Forum Focuses on Leadership in Radiology
Making Scans Easier for Smallest Patients, CHB Invests in Portable CT
Deficit Reduction Act Curtails Purchasing
by Renee Diiullo
Acquisitions slow in response to DRA as facilities carefully weigh need, volume, capacity, and cost.
The Deficit Reduction Act (DRA) of 2005 aims to cut approximately $40 billion from the federal spending program. According to the American Healthcare Radiology Administrators (AHRA), Sudbury, Mass, $11 billion of these cuts will come from Medicare and Medicaid and imaging will account for about one quarter of these health care savings. Outpatient services have been affected first, though many expect the new economics to eventually encompass inpatient services as well.
Therefore, the industry is watching how imaging centers are responding to the changes in reimbursement. The successful ones are taking hard looks at operations, efficiency, and performance. “Centers need to carefully scrutinize their budgets, pay attention to expenses, hire competent staff who can be cross-trained, and become as efficient as possible,” said Edward J. Cronin, Jr, CAE, AHRA’s executive director.
Although the first cuts vary with each center, acquisition budgets have been significantly impacted. Companies such as GE Healthcare, Waukesha, Wis, and Philips Medical Systems, Andover, Mass, have announced negative earnings impacts related to the DRA. “Institutions have to ask if a new technology is a want or a need. If it’s a want, it may have to wait until it’s a need,” said Richard Lewis, RTCRA, principal consultant for Phoenix Imaging Consultants, Orlando, Fla, and a member of the AHRA board of directors.
But even a “need” must still be tempered against the realities of volume, capacity, and cost. In addition to suffering reduced reimbursement rates, amounts for new technologies, such as multislice CT, have not yet caught up to expenses, and so new expenses are being minimized. “Acquisitions are slowing a bit, and, as imaging centers consolidate and partner with hospitals whose reimbursements have been less affected, they can be expected to slow again,” Lewis said.
That might mean longer life cycles for imaging devices. “Just because a piece of equipment depreciates over 5 years does not mean that you cannot try to use it for a longer period of time and extend its value,” Cronin said.
The disadvantage is that newer technologies often offer better images and marketing opportunities. “You want the best equipment for your patients so that you don’t miss anything but also for the competitive edge. You want to be able to say you have the latest and greatest,” Cronin said.
As more centers have to wait to purchase the latest and greatest, the latest and greatest may be introduced a little later. “While some companies and institutions will continue to push boundaries with faster and more efficient equipment, we will probably not see rapid acceptance of research and development technologies in the clinical world,” Lewis said. For instance, 64-slice may be the new gold standard for cardiology, but the wide adoption of 128-slice or 256-slice technology will be moderated by cost, volume, and capacity.
Hospitals will have to begin to consider these factors as well. Few expect that they will remain immune to cuts for long. “We are starting to see changes creep into hospital outpatient reimbursement,” Lewis said. The uncertainty affects acquisitions at these institutions as well since administrators do not want to commit funds that may not materialize. The effect on patients is still unknown.
“The jury is out on patient benefit. On one hand, the reductions force greater efficiency in operations, but in smaller facilities, such as those in rural locations, they may also force the closure of imaging operations, causing patients to travel further for associated procedures,” Lewis said. The deficit reduction has certainly impacted purchasing decisions; future effects remain to be seen.
Big Deal: Hospital Orders Carestream DR Systems
by Cat Vasko

|
| Illinois Valley Community Hospital uses the Kodak Directview DR 3000 System to conduct x-ray exams on its ambulatory patients. |
Illinois Valley Community Hospital, Peru, Ill, recently placed an order for two digital radiography (DR) systems from Carestream Health Inc, Rochester, NY. Illinois Valley selected the Kodak Directview DR 3000 and the Kodak Directview DR 7500 for their advanced image quality and convenient user interface.
“The company’s DR systems came out on top in our comparison of image quality, speed and ease of use, as well as service and support,” said Cindy Herrmann, the hospital’s administrative director of diagnostic imaging.
The hospital also invested in the Kodak Directview Capture Link system, which links Directview DR and CR systems, integrating CR images with DR studies and enabling cassette processing and image review at any CR system.
“The consistent user interface between the new DR systems and our existing Kodak Directview CR systems will help improve staff productivity and reduce training time,” Herrmann said. “The company’s history of outstanding service at our facility was also an important factor in our decision.”
According to Herrmann, the hospital will use the DR 3000, a compact system, to conduct x-ray exams on its ambulatory patients, and will use the DR 7500 to capture exams for trauma patients. With these systems installed, she said, the hospital expects to handle its ever-increasing patient workload with just two x-ray rooms, reconfiguring its two existing additional x-ray rooms for other purposes.
ACR Forum Focuses on Leadership in Radiology
by Cat Vasko
The seventh annual forum of the American College of Radiology (ACR), Reston, Va, brought together leaders in radiology, hospital administration, public health, business, and government for a summit held on July 22-23 and designed to pinpoint ways in which the ACR and its partners can better nurture a new generation of radiology leaders.

|
| Arl Van Moore, Jr, MD, FACR |
“One of the big challenges in radiology today is the lack of—or a complete void in—systematic leadership training for those who want to and can lead in radiology,” said Arl Van Moore, Jr, MD, FACR, chair of the ACR Board of Chancellors. “We need to have a strong bench as radiology moves into the future. This year’s forum sets the stage for us to do just that.”
Moore continued by observing that others could easily regard radiology as a “disorganized specialty, and use this to their collective advantage. At a time when radiology is squeezed by external forces, the absence of formalized leadership training may leave the profession vulnerable to a crisis.”
One of the attendees, James Thrall, MD, radiologist-in-chief at Mass-achusetts General Hospital, Boston, noted that often in radiology published academics are favored for leadership positions, regardless of whether they have demonstrated the skills necessary to be a good leader. “A cultural shift is needed before people will widely accept professional leadership development in the profession in general and in academia in general,” said Thrall.
Kathleen Dunne Eggli, MD, head of radiology at the Penn State—Milton S. Hershey Medical Center, State College, Pa, argued that supervisors should be actively recruiting and cultivating leaders from “an underutilized pool of talent.”
“Don’t assume sometimes reserved women or minorities aren’t interested in being leaders,” she said. “Tomorrow’s leadership will and should be one of diversity.”
And Richard Gunderman, MD, PhD, vice chair of radiology and pediatric radiology at Indiana University, Bloomington, added that leadership is not a frequently addressed subject in academic meetings. “Radiology should set high goals, including that of leading medicine in leadership development.”
The Journal of the American College of Radiology will publish a comprehensive white paper on leadership, authored by Gunderman and relating specific recommendations from the 2007 forum, in January 2008.
Making Scans Easier for Smallest Patients, CHB Invests in Portable CT
by Cat Vasko
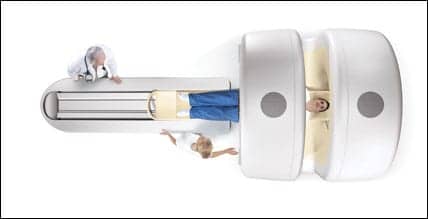
One of the leading pediatric hospitals in the United States, Children’s Hospital Boston (CHB), recently purchased a CereTom portable CT scanner from NeuroLogica Corp, Danvers, Mass. The CereTom is currently in use in the intensive care unit (ICU), and CHB plans to implement it in the operating room and radiology departments as well, facilitating rapid head, neck, and even full-body CT scans for neonates.
“The portability of the CereTom allows us to bring the imaging technology to the patient, rather than the other way around,” said Jeffrey Burns, MD, chief of critical care medicine at CHB. “We no longer need to transport some of these patients to the large hospital CT scanner, which is better for the patients and reduces the stress and anxiety for both patients and parents.”
Weighing in at just 800 pounds, the be-wheeled CereTom is light enough to be pushed from location to location within the hospital. “Or you can drive it like a powered lawnmower,” noted Eric Bailey, president and CEO of NeuroLogica. “It’s 29 inches wide; it will fit through any doorway. It consumes the power of your toaster oven in your house. We could plug it in in your kitchen. You can bring the device right to the point of care.”
This has ramifications for both pediatric and adult imaging. “We bring the device to ICUs to scan people without removing them from their life support,” Bailey said. “We can also bring it into the operating room. You can’t just bring a patient down to radiology in the middle of a surgery.”
At CHB, however, the CereTom is most useful in the neonatal ICU (NICU). “We bring our portable scanner right into the NICU room, put the [infants] on a kind of diving board, if you will—though it’s made of graphite in order to be x-ray lucent—and we scan them right there in a matter of 30 to 60 seconds and then get them right back in their incubator. That’s incredible for the health and welfare of the child.”
Also powerful is the ability to bring advanced 3D imaging to neonates. “On these little infants, radiologically speaking, they’re almost like a different species. All their little organs are crammed tightly together. One of these scans we did on a baby with a lung problem, and the doctors wanted to do a scan of the abdomen as well. They did an ultrasound and didn’t learn a lot. Did a CT of the abdomen and saw that the child’s whole intestinal system was disfigured. Seeing the doctors’ faces as they’re seeing the images in real time is incredible.”
The CereTom can also play a role in alleviating workflow problems, Bailey noted. “By locating a portable scanner in the ICU of the hospital, you limit transport [of critically ill patients to the radiology department] and all the costs associated with it, and you can do many more outpatient CTs on the big machine. Economically, what is demonstrated here is decompressing the big scanners. By taking these time-consuming patients off the big scanner, they’ve freed it up for more outpatients. And they make more money on the outpatients.
“We’re kind of like the pilot fish hanging on to the shark,” he summarized. “We actually make that big fish happy. We’re improving the efficiency of the big scanners and improving the workflow. And we’re also improving patient care.”