US Radiologists Exceed Established Mammography Practice Standards
39% of Physicians Expect to Limit Medicare Patients
Front Desk to Back Office: Radiation Oncology Software Improves Flow
Riverside Radiology Revisited
Ultrasound in Radiology in 2016: Projections and Strategies
|
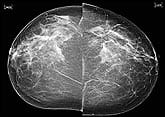
US Radiologists Exceed Established Mammography Practice Standards
Community mammography screening results surpass performance recommendations across the country, according to a study published in the October 2006 issue of Radiology1 that establishes performance benchmarks for screening mammography. The research—which was based on medical audit data funded by the National Cancer Institute (NCI), Bethesda, Md—examines the contributions of 188 mammography facilities, including results on more than 1.1 million women who underwent at least one screening mammography examination in the years between 1996 and 2002.
Key Findings |
|
Overall:
Performance Benchmarks for Abnormal Screening Mammographic Interpretations:
Performance Benchmarks for Cancer Detection:
* Positive predictive value (PPV) determined after a positive screening examination. |
The study provides, for the first time, contextual data against which radiologists can compare their mammography results. The pooled data from the study contains screening mammography interpretations determined by 807 radiologists. The current US breast cancer detection rate using mammography is 4.8 incidences per 1,000 women.
The researchers established performance benchmarks based on statistical analysis. The range of recall rate of the middle 50% of radiologists was 6.4% to 13.3%, and the range for 80% of radiologists was 4.4% to 16.8%, suggesting that radiologists often err on the side of caution. The range of PPV1 (positive predictive values determined after a positive screening examination) of the middle 50% of radiologists was 3.4% to 6.3%, and the range for 80% of radiologists was 2.6% to 8.6%. The range of PPV2 (postitive predictive values determined after a category 4 or 5 BI-RADS assessment) was 18.8% to 32.0% for the middle 50% of radiologists, and for 80% of radiologists, the range was 14.1% to 38.8%.
“The majority of radiologists appear to practice within the Agency for Health Care Policy and Research and European minimal guidelines for cancer detection rate and ductal carcinoma in situ detection, and the percentage of cancers that were classified as early stage appeared to substantially exceed the guidelines,” the report states. “These favorable outcomes are perhaps the result of the higher recall rates and/or shorter screening intervals that commonly are observed in practice in the United States.”
The report concludes by noting that many radiologists do not collect much performance data; however, efficient audit systems of screening mammographic practices are necessary for the collection of high-quality data, as well as the establishment of standards.
—C. Vasko
Reference
- Rosenberg RD, Yankaskas BC, Abraham LA, et al. Performance benchmarks for screening mammography. Radiology. 2006;241:55–66. Available at: radiology.rsnajnls.org/cgi/content/abstract/241/1/55. Accessed October 23, 2006.
39% of Physicians Expect to Limit Medicare Patients
The results are in from a 2006 questionnaire sponsored by the Medical Group Management Association (MGMA), Englewood, Colo. The June survey attained responses from 1,611 MGMA medical group practices representing more than 34,000 physicians; the average size of responding practices was 21 physicians.
As a result of changes to Medicare reimbursement made in the Deficit Reduction Act of 2005, what was the net impact on your reimbursement?
- No change: 21%
- Reduced 0.1%–5%: 57%
- Reduced 6%–10%: 10%
- Reduced 11%–25%: 3%
As a result of the scheduled reductions in Medicare reimbursement, what steps have you taken or do you plan to take in 2007?
- Cut administrative and support staff positions: 54%
- Cut clinical staff: 39%
- Cut staff salaries: 25%
- Modify or eliminate staff health care benefits: 67%
- Postpone investment in new technology: 80%
As a result of scheduled reductions in Medicare reimbursement of 5.1%, do you plan any of the following actions?
- Limit the number of Medicare patients seen: 39%
- Refuse to accept new Medicare patients: 19%
Front Desk to Back Office: Radiation Oncology Software Improves Flow
Using practice management software improved efficiency and income at one Arizona facility
By Dana Hinesly
Until someone invents a to-do list that completes itself, the next best thing is one that writes itself. For freestanding radiation oncology centers—particularly those with multiple locations—tracking work that needs to be done and employee performance is vital to success.
About 4 years ago, Arizona Oncology Services (AOS), which provides radiation oncology services at 13 facilities in the Phoenix metro area and Yuma, Ariz, installed an enterprise practice management (EPM) system from NextGen Healthcare Information Systems Inc, Horsham, Pa. Along with its myriad of functionalities, the solution generates work logs specific to each employee. These task lists are updated every 24 hours and appear on the desktop after individuals log on to the system.
Exactly what the task is and to whom it goes are determined by management. Virtually every process or procedure that needs doing in a practice can be entered into the system and assigned as appropriate. Therefore, the solution touches every aspect of the business, starting when the patient checks in.

|
| Tim McKeough |
“Until we installed NextGen, the radiation technology therapists constantly would have to go back and forth to the waiting room to see if their patient had arrived,” says Tim McKeough, chief operating officer for AOS. To minimize the wait time, therapists often were paged, presenting concerns about patient privacy. The EPM changed that: Now when the front desk checks in a patient, the therapist’s schedule is updated to show that the person is waiting. “It seems small, but the therapists thought it was great because it saves them a lot of wasted time,” McKeough notes.
Such seemingly minute efficiencies can add up quickly, especially when extrapolated to all departments. Once the patient is on the books, a task is created for the individual responsible for verifying insurance and eligibility. This job is created in real time, so within 5 minutes of scheduling, whoever is assigned to that duty will see a new item on his or her work log. Conversely, should a patient cancel, the EPM would delete any related tasks from all involved task lists.
Not only does it begin the process more promptly, but the system also flags any inconsistencies overnight. An incorrect insurance number or provider ID will be returned—as a task—to the initiating clinic for further review. Errors are remedied before weeks’ worth of billing can be produced.
Adaptability Is Key
For McKeough, another big selling point of NextGen was its open design. “The architecture was huge, because I’ve worked with systems where it was expensive and time-consuming to get a custom report,” he explains. “If I really need a number, and I just can’t find a report in NextGen, I can get it from my IT group within a couple of hours, because the infrastructure is very user-friendly.”

|
| Arizona Oncology Services achieved a return on investment on NextGen’s software within 1 year. |
The tech team at AOS further capitalized on the welcoming structure of the software by developing a “patient estimator” program, used during consultations with patients about to begin treatment. The patient estimator accesses the record kept in NextGen and gathers all of the contract information from the insurance carrier for that patient. After entering the CPT codes expected to be billed during the course of treatment, an estimate is generated informing patients of the total charges and how much they will be responsible for paying.
Assessing expenses in this way works in reverse as well. “We are doing a better job of letting patients know what their balance is going to be, so it’s very easy for us to sit down and counsel them,” McKeough says. “On the flip side, we also can set up a payment plan and, hopefully, not have to send out any statements.”
The Bottom Line
In addition to minimizing the number of statements generated, the software system has noticeably increased the productivity of AOS’ billing professionals. The company has cut the number of days required to collect on outstanding accounts almost in half. Accounts receivable averages less than 40 days now, as compared to around 75 days prior to the new system’s installation. Part of the savings came from speeding the time it took to get bills out the door.
“When I first came in, I did a date-of-service to date-billed analysis, and we were running, on average, 15 to 20 days to deliver the bill,” McKeough says, noting that the NextGen system makes it easy to bill. When the patient walks out the door, the therapist selects “bill it,” puts in the corresponding code, and saves. “Now, we’re running our date-of-service and our date-billed as almost the same day, so bills are going out 3 weeks faster than they were before.”
According to McKeough, the savings are realized in triplicate. Not only has the cash flow improved, but staff members spend less time entering charges and following up on unpaid invoices. In fact, staff productivity also is measured by the EPM. Once a task is assigned through the system, it must be acknowledged by being either completed or forwarded to a colleague. The software tracks when duties are put on a worklist, as well as when they are left unattended. Managers can create reports identifying who is doing how much and how quickly.
Having solid numbers and statistics removes all subjectivity and makes it possible for management to specifically address any issues, as well as dole out praise where applicable. “It not only gives us an idea of where we might be having a problem, but also where we might have a star performer, and it’s allowing us to put some bonus structures in place,” McKeough says. “It’s also easier for management to give people help, because in looking at what tasks are assigned every day, they can determine who might need assistance.”
The enterprise-wide facet means that tasks can be offloaded to others remotely, because all information resides on a central server.
Bang for the Buck
AOS realized a return on its six-figure outlay in less than a year, according to McKeough. Although the investment might not be feasible for smaller facilities, managing 24 doctors across 13 sites makes it well worth the investment.
“When we were in front of the executive committee trying to decide which system to buy, the analogy we used was that this is the Cadillac, not the Ford Escort, of practice management systems,” he says. “There are definitely cheaper systems out there, but you have to determine what means more to you—getting the functionality you want or saving a little bit more money.”
Dana Hinesly is a contributing writer for Axis Imaging News. For more information, contact .
Riverside Radiology Revisited
Three years later, the Columbus, Ohio, practice continues to thrive, and interventional radiology has been a key to its growth
By Tor Valenza
Riverside Radiology Associates (RRA) has had a dynamic vision since 1998 for how interventional services can dramatically build revenue and market share in the Columbus, Ohio, area. Axis Imaging News profiled the practice when its interventional office occupied a small suite adjacent to Riverside Methodist Hospital.1 Three years later, RRA represents the dominant interventional radiology (IR) force in the Columbus market. Since 2003, the group has developed its own 12,000-square-foot outpatient facility from which outpatient interventional services are performed; the group also has expanded IR coverage to five neighboring community hospitals with more hospitals on the way.

|
| From left are Riverside Radiology Associates’ co-medical directors Kevin McGraw, MD, interventional radiologist, and Thomas Lombardi, MD, body imager. |
RRA CEO Marcia Flaherty attributes the growth to three main factors: high demand for its outpatient services, innovative vascular and neurointerventional techniques for the new inpatient center located at Riverside Methodist Hospital, and constant physician outreach and education. Also, while demand is increasing for IR services in the Columbus area, RRA has few competitors in the interventional arena.
To quantify how much RRA has grown in the past 3 years, Flaherty points to comparable figures since 2003:
- The number of interventional procedures has grown 46%, helping to swell RRA’s total number of procedures from 360,000 in 2003 to more than 750,000 in 2006.
- The number of office visits has grown 88%.
- In 2003, there were seven interventional radiologists; throughout most of 2006, there were 10 interventionalists, and the group added three more in September for a total of 13; three more are sought.
- In 2003, RRA provided services at one hospital; today, RRA provides services at six hospitals across three health systems, and more facilities are within reach.
“The fact that RRA offers a complete package of services with extensive IR services was one of the key components in securing these new opportunities,” Flaherty explains. “These hospitals recognized the value of less-invasive, higher-quality, less-costly IR services and subspecialty diagnostic interpretations.”
Furthermore, RRA has increased the number of hospital procedures that it performs. The list now includes thrombolysis, aneurysm coiling, vertebroplasty, renal angioplasty, vascular stenting, and Merci clot retrieval.
12,000 Square Feet of Pain and Vein
Much of RRA’s increased IR numbers may be attributed to its new 12,000-square-foot outpatient center. The center is officially named Premier Medical Imaging; however, co-medical director, J. Kevin McGraw, MD, casually refers to it as “our pain and vein center.” Although that nickname might accurately describe the focus of the facility, it does not justly describe its 2 years of careful planning, spa-like setting, highly trained interventionalists, and brand-new procedure rooms. The center also offers a full range of outpatient diagnostic radiology procedures, including CT, MR, PET/CT, ultrasound, and nuclear medicine.
McGraw, an RRA partner and interventional radiologist, says, “We do some limited vascular access work there, as well as fistulagrams and angioplasty. But the predominant interventional procedures at our outpatient center are 95% pain- and vein-related.”
Premier’s upscale focus caters to self-paying clients who typically receive laser vein ablation and schlerotherapy. Most patients are women in their 40s who are covered by private payors, although a handful of patients are more than 65 years old and are covered by Medicare. Pain procedures predominantly performed at Premier are epidural steroid injections and vertebroplasty. These patients are primarily older than 65 and covered by Medicare.
Perhaps equally important to RRA’s success is its 10-month-old inpatient facility at Riverside Methodist Hospital. The new $5 million department was redeveloped in a former catheterization laboratory and features two flat-panel bi-plane neuro/OR suites from Siemens and two additional state-of-the-art angiography laboratories. The department includes a 12-bay holding area, spacious family waiting room, and a family consultation room.
The Brain Center
If RRA’s outpatient center can be called a pain and vein center, its inpatient center at Riverside Methodist might be referred to as its “brain center.”
Ronald F. Budzik, Jr, MD, a former instructor at Harvard Medical School, Boston, and neurointerventionalist at Massachusetts General Hospital, Boston joined the practice in 2002 and began developing a stroke program at Methodist, the first such program in the state to receive accreditation from Joint Commission on Accreditation of Healthcare Organizations. “He came to Riverside and was really able to pull together the multidisciplinary groups to develop a significant stroke program,” Flaherty says.

|
| Dubbed the “pain and vein center,” RRA’s new outpatient center, Premier Medical Imaging, features a spa-like atmosphere. |
Budzik works with the neurologist, the neurosurgeons, hospitalists, and emergency department staff, and physicians. He also is one of a few neurointerventionalists who participated in early trials for the Merci clot retrieval device for acute stroke patients. The cutting-edge procedure slips a corkscrew device into the artery, threads the corkscrew into the clot, and then pulls it out. “We have patients coming from throughout the state for the stroke treatment options that we offer,” Flaherty says. The center also coordinates with other emergency departments throughout Ohio for the efficient transfer of stroke patients to Riverside Methodist.
Budzik and Peter Pema, MD, RRA’s first neurointerventionalist and department chairman, visit many physicians and emergency departments throughout the local area, explaining their new procedures and how they can benefit patients. RRA’s expansion from providing services at two facilities to seven also is due to the group’s steady pace of education and outreach to the surrounding community hospitals. McGraw says that the group is always looking for new opportunities in the region, and because of RRA’s excellent reputation, opportunities often are looking for them.
“Smaller hospitals with five- or six-man diagnostic groups are constantly contacting us to provide the interventional services so they don’t have to worry about recruiting someone or having a part-time interventional radiologist,” McGraw says. Opportunities have developed at three small hospitals operated by Community Mercy Health Partners in the Springfield, Ohio, area, where RRA recently began providing diagnostic and interventional services. RRA is aggressively recruiting a core group of radiologists to live in the region. Currently, they have two.
In addition, Mercy and RRA have partnered to build a new outpatient center that should be finished in January 2007. The new Springfield center will include diagnostic imaging and IR services, such as the ones offered at Premier.
“It’s going to be an exceptional opportunity for residents of Springfield,” Flaherty says. “We have a great hospital partner who actually sought out our group to develop services with them. They’ve moved very quickly to build what will be one of the most comprehensive and outstanding outpatient centers outside of a hospital setting.”
Tor Valenza is a staff writer for Axis Imaging News. For more information, contact .
Reference
- Smith R. Admitting privileges. Axis Imaging News. 2003;16(4):16–21. Available at: www.imagingeconomics.com/issues/articles/2003-04_01.asp. Accessed October 23, 2006.
Ultrasound in Radiology in 2016: Projections and Strategies
By Cat Vasko
Members of the Society of Radiologists in Ultrasound (SRU), Reston, Va, convened in San Francisco on October 20–22 for their annual meeting. Before the meeting began, a 2-day conference, held October 17–18, focused on a more specific issue: Strategic Planning for the Future of Ultrasound in Radiology. Conference director Harvey L. Neiman, MD, SRU fellow and executive director of the American College of Radiology (ACR), Reston, Va, set the tone of the conference by urging radiologists to reach a consensus on how to “affect positive change and ensure a future for us in ultrasound 10, 20, 30 years from now.”
John J. Cronan, MD, FACR, radiologist in chief at Rhode Island Hospital, Providence, began the morning with an appraisal of radiology’s status in the ultrasound industry that reflected remarks made in his September 2006 Journal of the American College of Radiology editorial. Cronan listed current or potential threats to radiologists practicing ultrasound, including a shortage of radiologists, a lack of financial incentives for radiologists, the physician self-referral problem, and the increasingly popular notion that ultrasound is “the new stethoscope.”
“Everyone thinks they can perform ultrasound,” he said, “and the AMA has gone out of its way to say ultrasound belongs to all of medicine.” He mentioned a recent article in Forbes that referred to ultrasound as a “disruptive” technology—disruptive being a reference to its effect on the market—and comparing it to PCs overthrowing mainframe computer systems.
Neiman then returned to the podium to offer his perspective on both the “disruptive technology” issue and the issue of offshore outsourcing. Outsourcing, he noted, offers the same financial advantages in the medical field as it does in other businesses; and third-world radiologists tend to be far more adept than US radiologists at reading ultrasounds because they often are the only imaging technology to which they have access.
“What is the value-add that radiologists provide?” he asked. “If night-time outsourcing suffices, what is the value-add for daytime?” Adding to Cronan’s discussion of disruptive technology, Neiman noted that significant market forces demand the cost of health care come down, and democratized technology is one way through which it could do so. “Radiology must be alert to disruptive technologies,” he said. “Standing still is not an option for survival. I challenge you to decide what the value-add is that we bring to the industry.”
Vendor representatives then presented their companies’ ideas regarding where ultrasound technology is headed. Jim Brown, director of clinical and technical marketing for ultrasound at Philips Medical, focused primarily on the potential of volumetric imaging. “It changes visualization and the ability to quantify data,” he said, noting that new quantification technology could assist in volume measurements, volume automatic segmentation and analysis, regional and global motion analysis, functional volume imaging, and more.
Richard Chao, vice president of innovation at Siemens Medical, touched on the power of converged computing, storage, and communication technologies to facilitate: tissue equalization, acoustic coagulation, multimodality image fusion, computer-aided detection, and molecular medicine—all via ultrasound.
And Terri S. Bresenham, vice president and general manager of diagnostic ultrasound and IT at GE Healthcare, emphasized the potential of miniaturization. Workflow needs to improve considerably, she said—and faster, more compact technology can help. “It’s hard to lug around an MR or PET scanner,” she noted. “That’s where your stewardship of this should come in. This is the beginning of a renaissance period for ultrasound. I can’t think of a better technology to be in right now.”
Bruce Hillman, MD, took the stage to evaluate the state of the current research in the field. “As always, it’s really only about the money,” he said, explaining that he believes radiologists should focus on improving their ultrasound research and making the technology more meaningful to patients. He said the current research is not meaningful enough and suffers from a visible lack of critical thinking: “Case reports and case series are most of what we see, and they are inherently biased.” In his examination of 55 articles from the Journal of Ultrasound in Medicine (JUM), January through June 2005, he found that only three had extramural grant funding, 30 were retrospective, 32 would have been more accurately termed “case series,” none were multi-institutional studies, and very few articles even boasted a hypothesis. Beryl Benacerraf, MD, editor-in-chief of JUM, noted, “That talk was very optimistic about the time and resources we have to do research.”
Most exciting was the discussion of the technology’s potential to enable new procedures. Molecular imaging was the buzzword as radiologists like Barry Goldberg, MD, of Thomas Jefferson University Hospital speculated about the role of contrast agents in ultrasound by 2016. “The standard of practice in 10 years will be to give an injection of contrast, just as you do with CT and MR,” he predicted. “They say no one wants to work with contrast. I heard that [same complaint] when CT came out, too.” Early experiments with contrast-enhanced ultrasound have yielded 22% to 25% more diagnostic accuracy in animal models, and the therapeutic uses of injections are even more promising. Microbubbles and nanodroplets, safely encapsulating doses of pharmaceuticals until ultrasound aimed at a certain area breaks them open, have the potential to enable targeted therapy for tumors.
Opticoacoustics and elasticity imaging were two of the new applications that Jonathan Rubin, MD, professor of radiology at the University of Michigan and an SRU fellow, discussed in his talk. Photo-acoustic tomography has the potential to reveal brain function via scattered light absorption; the tiny temperature differences created by exposure to focused light create a measurable ultrasound wave. Rubin showed a slide of the effect of whisker stimulation on illuminated portions of a rat’s brain, demonstrating the possibilities of this real-time functional imaging. Elasticity imaging measures the hardness of tissue, helping track the development and age of arterial blood clots; strain is evaluated according to a simple formula involving the amount hard tissue expands versus the same measurement for control tissue.
James Borgstede, MD, chairman of the Board of Chancellors of the ACR, concluded the general session with a talk on ultrasound in the private practice setting, 10 years out and beyond. “Ultrasound can be saved,” he conjectured, “but not as we currently know it. The real question is, how will we advance this technology and its utilization for the benefit of our patients?” He listed a number of tactics that radiologists could and should take to reclaim ultrasound: halting the economic motivation to self-refer, supporting complete exams, interacting with patients, accepting quality competition, and marketing better to patients and to the referral base.
Borgstede noted research opportunities in the areas of contrast-enhanced ultrasound, targeted therapy, and fusion imaging. “You might be saying, woe is me, ultrasound is gone, it’s hopeless,” he told the group. “But I see this as a new dawn. We need to play offense.”
Cat Vasko is associate editor of Axis Imaging News. For more information, contact .





