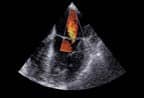
Women?s imaging is an area of complex modalities and rapidly emerging techniques. Dedicated training centers provide clinicians the opportunity to get comfortable with new procedures and products.

|
An old medical saying, popular in educational settings, goes, “See one, do one, teach one.” Dennis Wisher, RDMS, RVT, director of education and product management for Medison, Cypress, Calif, recalls how the adage applied to ultrasound about 25 years ago. Today, however, the saying no longer applies, particularly in imaging techniques across all modalities.
“The examinations and technology were much simpler back then, but today’s learning curve is longer,” Wisher said. Three-dimensional ultrasound, digital mammography, and breast MRIs represent significant differences from previous technologies and require more time to learn the nuances of each.
Subsequently, both proper training and experience are key to the successful acquisition and accurate diagnosis of medical images. Many companies in the discipline have always offered product training, but today, they are expanding their offerings to include comprehensive classes, simulated procedures, and online offerings.
“Regardless of whether the physician doing a particular procedure is a gynecologist, surgeon, or other clinician—whatever physician is performing a particular procedure—our goal is to make sure they have the necessary education to perform that procedure well,” said Debra Burnham, training center manager for Hologic Inc, Bedford, Mass.

|
Training often involves travel to a center where the distractions and interruptions common during regular practice are eliminated, and programs combine lecture and hands-on experience. Individuals are allowed to progress at their own pace, with some needing more practice than others to become confident with a procedure.
Naturally, physicians with more experience in the field tend to have shorter learning curves, and those less comfortable with computers may require a bit more time to become accustomed to the digital environment or new software, but generally, once a physician does become comfortable, he or she is excited to implement the new skills into practice.
Live and Learn
Physicians often seek training with the purchase of a new product or to meet CME requirements. “There are a few who come to training just for the credit, but I would say 99% come because they want to be better at what they are doing,” Burnham said.
Product training plays as important a role as experience in achieving that goal. “You have to understand imaging first and thereby understand what the product can do for you,” said Kamilia Kozlowski, MD, medical director and CEO of the Knoxville Comprehensive Breast Center in Knoxville, Tenn.

|
| Hologic faculty sometimes teach in small groups where participants provide their opinions about a case and then learn the actual findings. |
Knowing how a product and its features work can help to differentiate good imaging from bad imaging as well as improve diagnostic accuracy. Product training is key to obtaining this comfort level. “These are complex products that require expertise. They are used to make critical decisions for diagnosis and treatment, and incorrect use can lead to misdiagnosis and inappropriate treatment,” says Steven Harms, MD, clinical professor at the University of Arkansas for Medical Science in Little Rock, and a radiologist at the Breast Center of Northwest Arkansas with locations in Fayetteville and Bentonville, Ark.
Correct use often comes more quickly for those with past exposure to digital products. Those new to digital modalities, such as digital mammography, have to adjust to performing tasks electronically that they once did manually. “A radiologist who has been reading film mammography is often a little clumsy with the keystrokes when they first sit down and start interpreting digital images. They are used to manually picking up a magnifying glass or using a hot light, so that is initially the biggest challenge, but it only takes about a half hour and then they think it’s great. They can measure, window and level, and invert easily—features they haven’t had in the film world,” Burnham said.
New products generally also bring improved images with greater resolution, faster acquisition times, and more features that assist with image manipulation and interpretation. “Three-dimensional ultrasound will provide views of anatomy that are not attainable using conventional two-dimensional ultrasound, especially in women’s imaging,” Wisher said.
He notes that 3D ultrasound equipment can acquire an image of a full uterus within 3 seconds versus 10 minutes to 20 minutes using 2D. Three-dimensional ultrasound also can show multiplanar and volume views, such as the triangular shape of the endometrium. The tool is intended to complement conventional 2D ultrasound, not replace it, but it can be useful in confidently diagnosing patients at the point of care.
“Even though 2D and 3D ultrasound have many things in common, 3D does require a completely new skill set, and the sonographer or physician will need specific training,” Wisher said.

|
| Aurora’s dedicated breast MRI system was designed specifically with a woman’s anatomy in mind. |
Lesson Plans
Medison offers free 3-day training workshops taught by sonographers at its California facility to those who have purchased company productssnotes that off-site training removes complications associated with patient confidentiality and system integrity. The company opened the David Ellenbogen Center for Health Sciences Education at its headquarters to offer immersive training away from the “office.”
Hologic’s courses are designed around a particular procedure rather than a product. “The courses are educational so they are broad in their product scope, but the hands-on opportunities are product specific because we can’t offer all of the equipment that is out there,” Burnham said.

|
| The majority of Aurora’s training is done through simulated reads or procedures. |

|
The coursework starts with theory on the particular modality in question, but the majority of time is spent at workstations simulating reads or procedures. Cases are selected by the faculty and chosen to include some unusual results. The files are drawn from the instructor’s facility, or, if unavailable, Hologic will work with a site that has a large volume of patients to pull cases from which the instructor can choose. All cases are stripped of patient identifiers.
“Eighty percent of what physicians see is normal, and if they only do on-the-job training, they won’t see the abnormal cases and may miss them when they actually come across their workstation,” Culley said. But faculty can select cases designed to utilize the features of the workstation and to expose students to unusual cases.
The number of cases performed by each learning physician varies according to their experience and comfort level. “Some physicians will adapt quickly and feel confident after 25 or 50 cases. Others will read 80 or 100,” Burnham said. Physicians are able to print out their results versus the known truth and keep a record of the work they did.
Aurora Imaging Technology Inc, North Andover, Mass, also sees variety in the amount of necessary training for individuals. “We’ve got several hundred cases and have had a few people go through all of them, but I would say by the time they go through about 50, they are feeling pretty good,” said Harms, who is a member of Aurora’s faculty.
Kozlowski, who is an Aurora client and has taken its training, notes it is hard to measure when a clinician is done with training. “I think it takes years for any imager to become adept. Certainly the more you see, the more you learn. Even professors can be learning at the same time,” Kozlowski said.
Both Kozlowski and Harms equate product training to residency where the physician gets to practice with supervision. “Most people I train nowadays are people who do mammography. They understand breast imaging, the differential diagnosis of breast problems, and how to coordinate delivery with diagnostics and care, so I don’t need to cover those aspects,” Harms said.
He suggests that breast MRI users may sometimes benefit from some education in MRI physics, and therefore, Aurora’s classes also begin with didactic education, but the majority of training is done through simulated reads or procedures. Harms works up cases to mimic how they would be presented in actual practice and allows students to perform an interpretation that they then compare to Harms’ own as well as the final result. “You can go through 30 cases like that, and your confidence builds and you are able to do things more quickly,” Harms said.
Simulation doesn’t end with reads, however. Hologic and Aurora also offer coursework in procedures such as breast biopsy. The coursework walks students through the procedure step by step: how to interpret the image; how to find the suspicious area and why it is suspicious; how it should be biopsied; how to cleanse the area, numb the area, and use the device; and how to verify the right tissue was biopsied. “We simulate breast biopsy procedures with various meats, for instance, stereotactic with bologna and ultrasound with chicken,” Burnham said. An olive might represent the suspicious tissue. Aurora uses fruit. But whatever material is used, the physician often goes back to work ready to perform the procedure on his or her own.

|
| The larger portion of Hologic coursework is devoted to hands-on opportunities. |
Training in Action
Training is generally designed so that clinicians can take the knowledge back to the office and implement it immediately. “Implementation is interwoven through concept and theory, so users are introduced to clinical applications right from the start,” Wisher said.
Hands-on utilization reinforces that capability. Most educators believe it is key to enabling clinicians to successfully use the product in their practice. “Many times, people will see lectures, but unless they have a hands-on component with the system they have in their facility, it becomes too difficult for new users to try and incorporate what they’ve seen in the lecture into the real world,” Wisher said.
Burnham notes that the Accreditation Council for Continuing Medical Education requires follow-up 6 months after CME courses to determine the success of the training. The process includes precourse and postcourse surveys that inquire about where the individual is in the learning process before and after class and whether their skills have improved as a result of the training.
The Ellenbogen Center has now been open 7 months, and Burnham is beginning to receive follow-up surveys. “We are receiving high marks. People have found that the courses they’ve taken have shown a major improvement in their learning,” Burnham said.
Training, particularly that focused on mammography, can help physicians to make the right call. With the transition from analog to digital mammography, clinicians have the tendency to overcall. While this can prevent a missed malignancy, it also can result in unnecessary biopsies, which are costly for the system and worrisome for the patient. Unnecessary recalls tend to drop with experience.
“Readers can get the experience artificially by doing teaching cases where they view cases as if they were real, interpret those cases, and find out what the results really are. After you have gone through a few cases overcalling and undercalling a few things, then you develop a sense of what’s needed to make a quality diagnosis,” Harms said.
He suggests that what is needed in breast imaging may be the reverse of what the general radiologist is used to. “When I read whole-body MRI, I viewed the maximal intensity images last. Now, with a dedicated system, they are the first images I view,” Harms said.
Learning the New Way
Tips such as these help physicians new to a product or technique master it more quickly. Subsequently, the combination of lecture, hands-on training, and discussion has proven to be one of the more successful education methods. Wisher notes that hands-on workshops tend to facilitate shorter learning curves, and Burnham agrees.
“Whatever we can do to offer hands-on opportunities in small groups is the best thing, but the next best thing is small discussion groups,” Burnham said.
The faculty leads discussion on cases starting with what the students think the image shows and ending with what was done in the actual case. “The students get to think a little bit and are either right or learn another approach by someone with more experience,” Burnham said.
The Internet provides expanded opportunities, where students can continue to gain experience without having to travel. Physicians can read, hear, or view lectures and even practice reading cases. “The beauty of digital imaging is that we can transmit cases from one part of the world to another and discuss the case over the phone,” Kozlowski said.
Aurora offers MyPACS, a virtual teaching file and consulting space that users can turn to for education or decision support. “It’s a tremendous teaching tool because physicians have so many more cases to learn from,” Kozlowski said.
Conferences provide additional learning opportunities. Many companies offer training sessions and/or presentations at these events, which are designed to further attendee learning. As new technologies and procedures are introduced, training will play an even bigger role in clinician education. “There are a lot of new techniques coming out, particularly in women’s imaging, and physicians need lifelong training to keep up with these new technologies,” Culley said. That training will offer opportunities to see many and do many, and ultimately help many.
Renee Diiulio is a contributing writer for Medical Imaging. For more information, contact .