National surveys estimate a growing U.S. transgender population size along with increased recognition of transgender identity in the U.S. Gender affirming surgery is a treatment option for gender dysphoria along with counseling and sex/hormone therapy, and the utilization of such surgeries has been increasing.
“As gender-affirming facial feminization surgery (FFS) is increasingly performed for gender affirmation surgery for transgender women, so is preoperative planning computed tomography (CT). Radiologists have a key role in describing findings relevant to the surgical approach,” says Andrew Callen, MD, current assistant professor at the University of Colorado Anschutz Medical Campus, Department of Radiology (CU Radiology) and former clinical fellow at the UC San Francisco Department of Radiology and Biomedical Imaging. “Communication between radiologists and surgeons is key in ensuring the success of the surgery and the overall care of transgender patients.”
A team of radiologists and surgeons from the UCSF Departments of Radiology and Surgery – Division of Plastic and Reconstructive Surgery, CU Radiology and the Oregon Health Sciences University Department of Radiology (OHSU Radiology) recently collaborated on an article that describes the radiologist’s role in an important aspect of the care of gender diverse patients, namely preoperative FFS planning.
They focused on the bony craniofacial aspects of FFS preoperative planning, and described readily identifiable CT features with a key role in FFS planning. Dr. Callen was corresponding author on the article, recently published online in the American Journal of Roentgenology.
“Facial CT provides greater anatomic detail and improved 3D characterization of the face when compared to radiography, and CT imaging is involved in the routine preoperative assessment of the patient undergoing FFS, as well as postoperative imaging assessment if needed,” says Jared Narvid, MD, assistant professor at UCSF Radiology and an author on this study. “The article demonstrates how a radiologist can add value to image interpretation by reviewing the anatomic targets for surgical change, and the role of pre- and post-operative CT in these patients’ care with attention to commonly observed CT findings and pitfalls that surgeons use to determine the surgical approach.”
Overall, familiarity with these findings will facilitate improved communication between radiologists and surgeons, thereby contributing to the care of transgender women. What’s next? While the article highlighted the use of CT for the evaluation of the facial bones, the soft tissues of the face play an equally important role on surgical success. Future work may explore potential use of MRI in pre-operative planning of facial soft tissue as well as facial masculinization surgery or its radiologic considerations, both areas to be explored in the future.
Featured image:
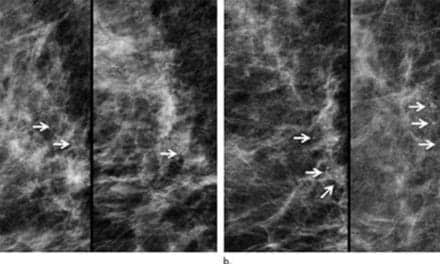
Figure 2: Pre- and post-operative CT in two different patients undergoing facial feminization surgery. Frontal 3D reformatted images (A) before and (B) after surgery in a 29-year-old transgender woman. Red dashed line indicates frontal bone osteotomy. Red dash-dot lines indicate mandibular angle osteotomies. Red solid line indicates genioplasty. Green arrowheads indicate superior orbital foraminal notches. Blue arrowheads indicate mental foramina. Sagittal reformatted images (C) before and (D) after surgery of 39-year-old transgender woman. Note the Osterhout type 1 frontal sinus. Red dashed line indicates frontal bone recontouring. Red solid line indicates genioplasty. The nasofrontal angle (yellow line) is increased postoperatively. (Courtesy: American Journal of Roentgenology)
Reference
Callen AL, Badiee RK, Phelps A, et al. Facial Feminization Surgery: Key CT Findings for Preoperative Planning and Postoperative Evaluation [published online ahead of print, 2020 Dec 30]. AJR Am J Roentgenol. 2020;10.2214/AJR.20.25228. doi:10.2214/AJR.20.25228