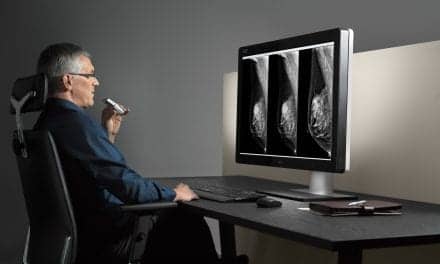
In pediatric scoliosis treatment, the latest imaging technologies are helping clinicians to reduce radiation exposure, more efficiently diagnose, and plan surgeries.

|
The next generation of scoliosis imaging tools has arrived, slowly working their way into hospitals and imaging suites. Although more expensive, this new generation in scoliosis imaging can help radiologists and orthopedic surgeons to perform the same tasks more efficiently and with less radiation exposure to their young patients.
Until recently, little has changed in imaging tools for pediatric scoliosis patients. Protocols for monitoring scoliosis typically require one—often several—x-rays per year, exposing young children and teenagers to multiple doses of radiation. With film x-rays, technologists would then manually marry two sectional films together in order to see the erect anteroposterior and lateral views of the entire spine. Physicians would then take 20 or 30 minutes to calculate the degree of curvature with the Cobb method, utilizing the low-tech—but effective—pen and ruler.
While these methods are all valid and still very much in use today, orthopedic surgeons and hospitals upgrading their imaging suites are gradually turning to more modern methods that utilize new technology, such as various digital radiographic systems, which emit lower doses of radiation and stitch together separate radiographs, plus new software that helps surgeons navigate through spinal procedures.
Reducing Radiation Exposure
Physicians have long been concerned about the radiation doses being absorbed by young scoliosis patients. Thyroid, breast, ovaries, and other tissues are especially susceptible to cancer risks from radiation.
“Spine x-rays are going to radiate several radiosensitive tissues, and we are doing our best to minimize that exposure,” said Peter O. Newton, MD, director of scoliosis service and orthopedic research and chief of surgery at Rady Children’s Hospital in San Diego.
One of the low-tech and low-cost ways that Newton and others are reducing radiation dose is by imaging patients from the posterior-anterior (PA) view rather than the anterior-posterior (AP) view, thereby reducing the direct exposure to tissue-sensitive areas in the front of the body, such as the breasts. In addition, physicians are employing relatively inexpensive filters and clear lead shields that are protecting the sensitive tissues from radiation without degrading image quality of the spine.
As hospitals and physicians upgrade their radiology suites, pediatric scoliosis patients are also benefiting from CR and DR systems that emit less radiation than analog film technology.
However, even these modern systems still expose children to more radiation over the course of many years than clinicians would like.
“Even at what we typically consider low doses, the bad carcinogenic effects of radiation, that’s all cumulative over time, especially for the pediatric deformity kids,” said Gordon D. Donald, MD, director of spinal surgery, New Jersey Spine Group, Eatontown, NJ. “We’re doing 20, 30 x-rays over the course of several years when treating those patients, so it becomes a big number in their total radiation exposure.”
When Donald decided to upgrade his equipment and remodel his practice, he considered a more traditional CR system, but instead chose a new ultralow-dose orthopedic x-ray imaging solution called “EOS” from Marietta, Ga-based Biospace Med USA.

|
| The EOS is able to quickly perform a full digital pediatric scoliosis workup without film cassettes, film stitching, or time-consuming positioning of patients. |
Biospace USA’s parent company is actually European, and its EOS system has been in the European market for several years now. Donald’s New Jersey Spine Group is the first facility to install the American version that was recently cleared by the FDA.
According to Biospace, EOS can reduce radiation by as much as 10 times less than a conventional x-ray system and up to 1,000 times less than a CT scan.
The EOS system is unique to conventional systems in several ways. First, it is a self-contained x-ray chamber that requires no external lead shielding in the walls of the Spine Group’s new offices.
More significant is the way that EOS is able to quickly perform a full digital pediatric scoliosis workup without film cassettes, film stitching, or time-consuming positioning of the patients. Children simply walk into the EOS chamber and stand on a predetermined spot on the floor. From there, multiple sharply focused x-ray beams quickly image the spine or the entire patient from head to toe in seconds.
Donald explained, “Instead of taking one shot that covers a region, EOS takes hundreds of shots that shoot straight parallel across. It’s very much like a linear CT, but instead of being circular like the CT, it does it in a linear fashion. The mechanism goes up on a worm gear, so it takes hundreds of perfectly focused layers, and then the computers stack them together.”
Donald said that aside from the lower radiation doses and sharper images, the system is efficient because EOS simultaneously acquires both the AP and lateral views with one exam.
“That makes the result so much more accurate from the comparison of one study to another, done months or years later,” he added.
Naturally, all of this sophisticated technology comes at a cost, perhaps 1.5 to two times as much as a more conventional CR suite, according to Donald. But he said that aside from the clinical benefits to patients, he saved in construction costs because the EOS unit is self-shielded. Technologists also will be saving a significant amount of exam time.

|
| Orthoview provides templates to measure vertebral centroid, sagittal balance, apical vertebral translation (AVT), thoracic and lumbar curves, sagittal alignment, and others. |
New Orthopedic Software Tools
Of course, EOS will have to compete with the CR and DR systems that dominate the market today. CR systems have a wide selection of vendors who offer software tools that can splice top and bottom x-rays together and quickly incorporate them into PACS.
Some of these tools have better alignment capabilities between top and bottom studies. Other systems can have better or worse heterogeneity of the gradation of brightness, so that bone density among the images may appear to be slightly off color.
Nevertheless, many of these issues can be manually adjusted and are certainly more efficient than stitching together and importing cassette-based film studies into PACS.
Beyond CR splicing technology, orthopedic surgeons are also enjoying the benefits of new software that provides templates to measure the Cobb angle and other orthopedic measurements.
Cedara software from Milwaukee-based Merge Healthcare; Germany-based Hectec; Jacksonville, Fla-based Orthoview; and Traumacad, a Tel Aviv-based company, all offer these advanced orthopedic surgical planning tools.
Todd A Milbrandt, MD, assistant professor of orthopedics at Shriners Hospitals for Children, Lexington, Ky, uses the Orthoview software for his practice and sees it as a huge step forward over using plain film and a pencil for angle measurements.
“In scoliosis, it’s basically all about a Cobb angle, which isn’t super complicated to do without Orthoview, but they’ve added things recently that we’ve been working with the new viewer to give us more adaptability.”
Aside from the Cobb angle measurement tool, Orthoview provides templates to measure vertebral centroid, sagittal balance, apical vertebral translation (AVT), thoracic and lumbar curves, sagittal alignment, and others.
Milbrandt estimated that the Cobb angle tool alone saves him 20 to 30 minutes for every patient. He also uses the program for nonspine-related applications, such as measuring limb-length angulations.
“Before, we had to measure them out on long, plain x-ray films. Now, they’ve come up with templates that allow us to put a circle on a femur head and add a line down to the knee and a line down to the ankle, and then it calculates all of those angles automatically.”
Milbrandt noted that while the software does not help him with the surgery itself, it is a great help in the clinic. “It helps me see many of these patients quicker and more efficiently,” he said, “and it stores those images where I don’t have to worry that the marks that I’ve made are going to wear off.”
3D X-ray Reconstruction
Another tool that may help plan scoliosis surgeries and better define deformities will be x-ray three-dimensional (3D) skeletal reconstruction from the two simultaneous planar images generated by the EOS system. Like the 2D tools, the EOS software will provide automatic measurement software designed to calculate a variety of measurements and angle calculations between individual bones and joints, but in 3D.
The software will be unique to the EOS system because of its multi-x-ray system. However, as of this writing, it is available only in Europe and Canada and is awaiting FDA clearance.
Daniel W. Green, MD, associate professor of orthopedic surgery of the scoliosis service for the Hospital for Special Surgery, New York, has only heard of the product, but is intrigued by the 3D potential.
“There’s certainly more awareness of the 3D rotational deformities that go along with scoliosis,” Green said. “In some of our most severe scoliosis, we’ll get chest 3D imaging to see the lungs, the thoracic cage, to try to get a better handle on what the rotational malalignment of the vertebrae is.”
Green also noted that surgeons are increasingly using more pedicle screws in scoliosis surgery, including in the thoracic spine. As a result, many orthopedic surgeons are obtaining more 3D imaging to evaluate the anatomy in order to assist with the presurgical planning and placement of those screws.
Newton of Rady Children’s has performed some evaluation of the EOS 3D system while working with researchers in Montreal at St. Justine Hospital.
“We traditionally image [scoliosis patients] with upright plane radiography with AP and lateral views. This tells us a lot about the deformity, but it is difficult to integrate into all three planes—particularly the transverse plane. So having the ability to have a system that will allow us to view all three planes of the deformity is extremely important in our understanding of the deformity in ways that we haven’t really been able to see the deformity.”
Newton hopes that the EOS 3D studies may reveal different ways to classify the deformities and uncover new ways to describe the magnitude and the severity of the deformity. Presently, that is done almost exclusively on the PA radiograph with the Cobb angle.
“[The Cobb Angle] is certainly one of the most important measurements of scoliosis, but it may not be the most representative,” Newton said.
Newton also pointed out that the EOS 3D reconstructions are not the same as a CT reconstruction. “You have to understand the limitations of what you’re getting. You’re getting an estimate of outer shell of the shape of the vertebra and that global deformity of the spine, rather than specific detailed three-dimensional anatomy that we are used to getting in a 3D CT scan.”
Newton looks forward to the technology being approved, but said that it is too soon to tell whether having this extra 3D view will improve outcomes. “How we interpret that three-dimensional understanding still remains to be known. It is logical to think that the better understanding you have of a deformity, the better you will be able to treat it, but we have been operating without all of that information to date.”
Donald has also evaluated the product and is optimistic about its potential. He said that much scoliosis deformity involves rotation and tilting of individual vertebra, but until now, there has not been technology that measures the degree of those deformities.
“You can’t just look at plain x-rays to be able to measure these things. That’s where the 3D reconstructions come in. They give us perfect measurements of each vertebral rotation, of each vertebral tilting. As your instrumentation becomes more specific, to be able to address these pathologies, we now have a way to not only measure it, but to follow it and remeasure it after surgery and better understand what we’re doing during our surgery,” Donald said. “So with that added information, we’re absolutely going to be able to do a better job in the future.”
Tor Valenza is a staff writer for Medical Imaging. For more information, contact .