 |
by Cat Vasko
· Study: CAD for Breast MRI Improves Standardization and Analysis
· Tech Zoom: I-Response Monitors Effects of Cancer Therapy
· Research Alert: IMDS Releases CTLM Clinical Study Results
· Research Alert: ACR Won’t join National Accreditation Program for Breast Centers
· High Dose of Chemo Adds to Lung Cancer Survival Rates
· Education & Research: SNM Awards $105,000 in Grants
Study: CAD for Breast MRI Improves Standardization and Analysis
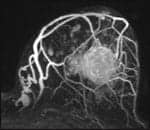
Research published in the July issue of Radiology indicates that computer-aided detection (CAD) for breast MRI may improve both standardization of studies and the analysis of benign and malignant lesions. In “Breast MR Imaging: Computer Aided Evaluation Program for Discriminating Benign and Malignant Lesions,” lead author Teresa Williams, MD, and colleagues at the Seattle Cancer Care Alliance and the University of Washington Medical Center, Seattle, used CADstream 3.0 from Confirma Inc, Bellevue, Wash, to examine 154 breast lesions deemed suspicious by radiologists that were visible only on MRI and had been biopsied under MRI guidance.
|

|
| New research indicates CAD improves analysis of benign and malignant lesions. |
The lesions in the study had been identified and biopsied during 2001-2004 from a study population of 125 women, ages 27-86. CADstream marked the areas where the MRI data curves were characteristic of abnormal lesions, and analysis of the tissue enhancement data as displayed in the CAD-processed images identified 38 of the 41 malignant lesions examined by radiologists using the software, according to researchers. Using the standardized CAD protocols and enhancement profiles, the radiologists also noted a reduction in their false-positive rate.
“What’s striking is how few people are comfortable with breast MRI,” said David Gruen, MD, a radiologist at the Norwalk Radiology Center, Norwalk, Conn, who works with CADstream regularly. “It’s my feeling, after doing this for multiple years both with and without CAD, that if you’re doing a lot of breast MRI—and you need to do a lot to do it well—it’s hard to imagine doing it well without a program like this. Each case generates between two and three thousand images. Try finding the needle in the haystack with something like that. No wonder it’s daunting. No wonder people are reluctant to get into this business.
“On the other hand,” he continued, “with CAD, it’s a breeze. All the post-processing is done behind the scenes. The computer puts a huge amount of data into a very usable format. The time to interpret goes down significantly, and that takes away anxiety.”
Constance Lehman, MD, corresponding author and director of radiology at the Seattle Cancer Care Alliance, noted that the computer did not detect benign lesions the majority of the time. “There was a very small risk of a false negative from the CAD program,” she said. “But it also didn’t flag lesions that were benign. So it might have the potential to reduce the false positives associated with MRI. We have to be careful and remind ourselves that we’re relying on the radiologists’ assessment of every lesion; however, there is no CAD program that’s 100%.”
In the study, Lehman and colleagues evaluated how the CAD program detected changes in contrast intensity over time, with encouraging results. “Contrast was addressed first because one of the biggest challenges in breast MRI is interpreting multiple exams over time,” she said, echoing Gruen’s sentiments. “Breast MRI CAD significantly decreases false-positive exams.”
“The biggest challenge to breast MRI has been that it’s very sensitive, but not very specific,” Gruen noted. “The sensitivity approaches 100% for lesions of 3 to 4 mm. We’re also finding 90% of ductal carcinoma in situ. But we need the specificity. If you can stop finding those benign lesions, you’ve hit a home run. And that’s what this article shows you can do.”
Gruen tempered the success of the CAD program with a sobering note, however. “We sometimes need to separate the individual person’s risks and concerns from what we recommend as a society,” he said. “As a society, we can’t afford to biopsy every lesion. But when it’s done well, we’re going to find a lesion that we wouldn’t find any other way. The American Cancer Society’s mission is saving lives on a community basis, and ours is to save lives one at a time.”
Tech Zoom:
I-Response Monitors Effects of Cancer Therapy

|
On May 22, medical device manufacturer Endocare Inc, Irvine, Calif, announced that a randomized clinical trial of 244 men with localized prostate cancer showed that cryoablation was at least as effective at treating the disease as external beam radiation. The study was the first North American clinical trial in 25 years to enroll more than 100 patients for its comparison of two definitive prostate cancer treatments.
Another interesting finding shows that 6.6% of the cryoablation patients had positive biopsy findings after 36 months?compared with 26.3% of the patients who underwent radiation therapy. Results of the trial were presented by leader Bryan J. Donnelly, MD, a urologist at the University of Calgary, at the annual meeting of the American Urological Association (AUA), Linthicum, Md.
“This study demonstrates that cryoablation is equivalent to external beam radiation when used to treat localized prostate cancer,” said Donnelly. “Furthermore, the positive biopsy rates 3 years after treatment were significantly higher for patients who underwent radiation therapy. A positive biopsy alerts a physician to recurrent or residual disease within the prostate and indicates that additional treatment may be necessary. Like radiation therapy, cryoablation is a treatment option that should be considered by all patients who are diagnosed with localized prostate cancer.”
Cryoablation was the subject of three other studies presented at the conference, and the AUA is offering a number of postgraduate courses and workshops featuring training and information on the use of cryoablation.
“The continued production of quality data by leading physicians and the presence of AUA-sponsored cryoablation courses at this year’s annual meeting mark the emergence of the cryoablation technology in the mainstream of urology,” said Endocare CEO Craig Davenport, “and indeed all areas of medicine where minimally invasive treatments for cancer are needed.”
—Cat Vasko
Research Alert:
IMDS Releases CTLM Clinical Study Results
In June 26, Imaging Diagnostic Systems Inc (IMDS), Fort Lauderdale, Fla, released select results from a study on the advantages of using computed tomography laser mammography (CTLM) as an adjunct to conventional mammography to improve detection of occult cancers in dense breasts. The results were published in full in volume 16 of the journal European Hospital.
“We’re using the patient’s own blood as a contrast medium,” summarized Eric Milne, MD, IMDS director of clinical research and professor emeritus of radiology and medicine at the University of California, Irvine. “At the wavelength we use, there’s almost no absorption by water or fat. Dense breasts contain a great deal of water and are therefore difficult [to image] for conventional mammograms. The sensitivity of conventional mammography in dense breasts is only about 30%. But the dense breast does not affect our laser beam, so we have much higher sensitivity.”
The original study was performed on about 750 women, but that number is increasing all the time as IMDS works to further clinically validate the technique. “It’s gone up to about 9,000 women all over the place—Beijing, Dubai, Poland, Italy, and so on,” Milne said. “We’re focusing primarily on women with dense breasts. That’s a huge problem with mammography. We don’t need a lot of help in fatty breasts. About 40% of women have dense breasts, but that varies from country to country; for example, in China the percentage is much higher, whereas in Poland the reverse is true—breasts tend to be large and very fatty.”
Milne explained that the ideal study would look only at dense breasts, but because a mammogram is required to learn whether a breast qualifies as dense, assembling a patient base essentially amounts to a numbers game. There is a large study under way at six different US breast centers, the results of which will be shared with the FDA.
“At the moment, CTLM has to be an adjunct, even in the dense breast, because you don’t know whether the breast is dense until you do a mammogram,” Milne noted when asked about the technology’s potential following successful FDA approval. “But mammography only shows morphology. You also need to look at function, and angiogenesis is one of the primary functions of a tumor.”
And absorption imaging represents only half the promise of CTLM. The second is fluorescence imaging. “All around the world, people are trying to find what’s specific to breast cancer—a gene, a protein, an enzyme,” Milne said. “When you find that, you attach something luminescent to it and inject it in the patient. Then you do CTLM, record it on the fluorescence detector ring, and you’ve got a yes or no answer. What angiogenesis does not do is tell you whether the tumor is benign or malignant, but that answer is just around the corner.”
Which, in a world where 80% of breast cancer biopsies turn out to be false positives, is a powerful possibility. “Unnecessary biopsies happen to be huge in the United States at the moment,” Milne noted. “It’s terrifying for women.”

|
Research Alert:
ACR Won’t join National Accreditation Program for Breast Centers
On June 28, the American College of Radiology (ACR), Reston, Va, announced that it will not be participating in the National Accreditation Program for Breast Centers (NAPBC). Also abstaining from participation in the initiative, which members of the American College of Surgeons (ACS), Chicago, first proposed is the Society of Breast Imaging (SBI), Reston, Va. The NAPBC is a voluntary program administered by an independent multidisciplinary board comprised of members of various medical organizations involved in the delivery of care in a breast cancer setting.
The ACR and the SBI have been involved in discussions with the organizers of the initiative for 2 years. However, the ACR said in a statement, “We have been unable to reach agreement with this body over the incorporation of the ACR’s long-established standards, practice guidelines, and accreditation programs related to breast imaging and image-guided interventions, despite the fact that these programs do not exclude participation by practitioners of specialties other than radiology.”
The ACR and the SBI maintain that in order to ensure quality care in the breast center setting, the other specialties involved need to establish and validate standards for themselves comparable to the standards developed by the ACR for breast imaging.
The ACR plans to introduce a similar voluntary initiative this fall called Breast Imaging Centers of Excellence (BICOE); facilities meeting certain criteria will receive the designation. BICOE and the NAPBC will not be mutually exclusive.
High Dose of Chemo Adds to Lung Cancer Survival Rates
A study in the July 1 issue of the International Journal of Radiation Oncology*Biology*Physics reports that patients with inoperable non-small cell lung cancer (NSCLC) who receive an initial high dose of chemotherapy prior to treatment can expect an increase in overall survival. The boost of chemotherapy is known as induction chemotherapy; physicians administer the medicine to stop the growth of the cancer in the lungs and prevent it from metastasizing to other parts of the body, as sometimes happens in patients with NSCLC.
The study was conducted at the MD Anderson Cancer Center, Houston, where 265 patients with inoperable NSCLC were divided into two groups. One group, containing 127 patients, received the induction therapy and the chemoradiation; the second group, which contained 138 patients, received only chemoradiation.
The chemoradiation method used on all 265 patients included 3D conformal radiotherapy and concurrent chemotherapy, which, the study’s authors reported, generally consisted of a weekly platinum- and taxane-based regimen, weekly platinum and etoposide, or cisplatin and etoposide for two cycles. Radiation treatment typically targeted the gross tumor volume and the involved lymph node stations; uninvolved lymph node stations were not effectively irradiated.
The 127 patients chosen for the initial high dose of chemotherapy were treated for two or three cycles using a dual-agent regimen; the majority was treated with platinum and taxane-based regimens, while six patients received cisplatin and etoposide, cisplatin and gemcitabine, or gemcitabine and vinorelbine. The decision to undergo induction chemotherapy was determined by the patient and their physicians.
The researchers found a small, but statistically significant, increase in the overall survival rate of patients who received the induction therapy. The 127 patients showed an increase in survival by an average of 6 months compared with the control group. The rates for distant metastasis-free survival were also higher for the induction group, with a success rate of 42% at 5 years, compared to 23% in the chemoradiation-only group.
The researchers noted in the study that “an unknown number of patients may have been initially started on induction chemotherapy with the intent of proceeding on to definitive concurrent chemoradiation, but subsequently did not receive concurrent chemoradiation owing to early development of metastatic disease during the induction chemotherapy.” Because the study is retrospective, these patients could not be identified for inclusion in the study population; however, the researchers added, “to evaluate whether this potential selection bias may have affected our results, we repeated our analysis but excluded any patient from the without-induction-chemotherapy group who had an early distant metastasis or early death within 2 months after finishing concurrent radiation.”
Further retrospective analysis showed that patients with the cancer subtypes of adenocarcinoma, or large cell carcinoma, benefited the most from induction chemotherapy, whereas those with squamous cell carcinoma did not.
“Studies like ours challenge traditional methods for treating cancer, while still preserving and building on what has already been established as effective in the treatment of lung cancer,” said Eugene H. Huang, MD, radiation oncologist at MD Anderson and lead author of the study. “This study raises questions about how we approach our treatment processes, and further research will be needed to find the best way to increase survival in these patients.”
Education & Research
SNM Awards $105,000 in Grants
The Society of Nuclear Medicine (SNM), Reston, Va, recently awarded a total of $105,000 in research grants and fellowships funded by its Education and Research Foundation. “By funding scholars so they may pursue independent research projects, SNM continues its long-time tradition of promoting the discovery of new science and the creation of new techniques and technologies,” said Mathew L. Thakur, chair of the Society’s Awards Committee.
Steve Shih-Lin Huang of the Cleveland Clinic, Cleveland, Ohio, won the $25,000 SNM/Mallinckrodt Seed Grant in Molecular Imaging/Nuclear Medicine Research for his research in three-helix-bundle ribosome display systems for VEGRF2 imaging. Monica Sala-Rabanal at the University of California David Geffen School of Medicine, Los Angeles, was the recipient of the $10,000 Mitzi and William Blahd, MD, Pilot Research Grant for her project studying the functional expression of glucose transporters. Xuping Zhu of Brigham and Women’s Hospital, Boston, received the $10,000 Mallinckrodt Pilot Research Grant for the study of quantitative Y-86 PET imaging for monitoring Y-90 therapy.
Additionally, SNM awarded five pilot research grants, each totaling $8,000, to support clinical and basic research by young investigators interested in testing innovative ideas while other major grant support is being sought. Five $3,000 Bradley-Alavi fellowships were awarded to students participating full-time in clinical and basic research activities in the area of nuclear medicine.
Finally, the prestigious Mark Tetalman Award, which honors the work of a young investigator pursuing a career in molecular imaging and nuclear medicine, was presented to Matthew A. Kupinksi, an assistant professor in both the College of Optical Sciences and the Department of Radiology at the University of Arizona, Tucson. Kupinski’s research interests include task-based assessment of image quality for both tumor detection and parameter estimation tasks, understanding the statistical characteristics of images and objects being images, imaging hardware optimization, and human-observer models for image analysis.
“It is a great honor to be recognized by SNM and receive this award for my work,” Kupinksi said.
—Cat Vasko





